What Are Grounding Techniques? 11 Ways To Calm Anxiety
Your heart races. Your thoughts spiral. The present moment feels impossibly far away. If you’ve experienced anxiety, panic, or the aftermath of trauma, you know this feeling. So what are grounding techniques, and how can they help? These are practical tools designed to interrupt that spiral and bring you back to the here and now.
Grounding techniques are simple, evidence-based strategies that redirect your focus from overwhelming emotions to your physical surroundings and bodily sensations. They engage your senses and anchor you to the present, skills that prove especially valuable for managing anxiety, panic attacks, and trauma responses.
At Trellis Counseling, we teach grounding techniques as part of our trauma-informed therapy practice in Oregon. These exercises support deeper healing work, whether you’re processing difficult experiences through EMDR or building emotional regulation skills in individual sessions. This guide covers 11 practical grounding techniques you can start using today, from the well-known 5-4-3-2-1 method to physical and mental exercises that calm your nervous system when you need it most.
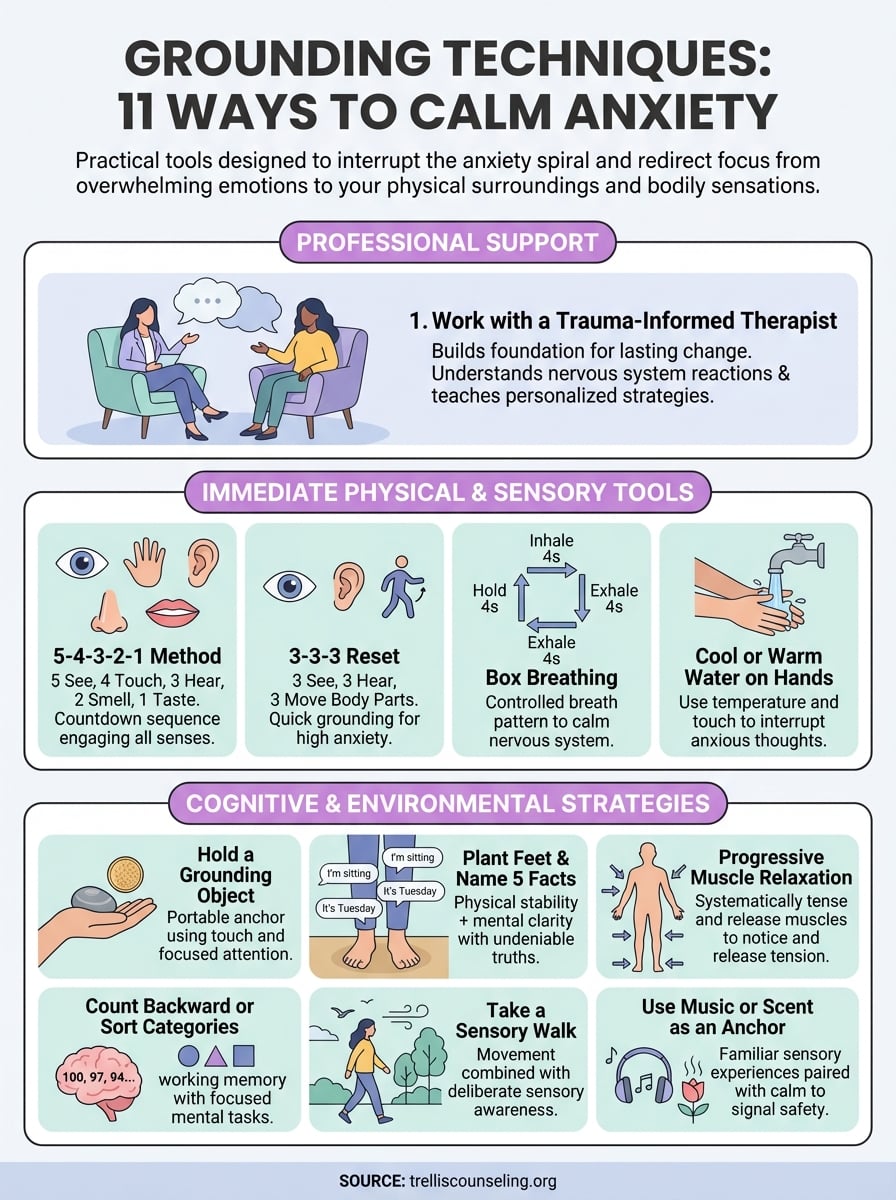
1. Work with a trauma-informed therapist
While you can practice grounding techniques on your own, working with a trauma-informed therapist provides the foundation for lasting change. A trained professional helps you understand why your nervous system reacts the way it does and teaches you personalized strategies that address your specific triggers and needs.
What it is
Trauma-informed therapy recognizes how past experiences shape present reactions. Your therapist creates a safe space where you learn about your nervous system’s response patterns, practice regulation techniques, and develop personalized grounding strategies that work for your unique situation. This approach acknowledges that trauma affects how you process stress and anxiety, requiring specialized skills beyond standard counseling methods.
How it supports grounding skills
A therapist teaches you which grounding techniques match your nervous system state. You learn to recognize early warning signs of dysregulation and select appropriate exercises before panic escalates. Your sessions provide a safe environment to practice these skills while receiving immediate feedback and adjustments. Professional guidance helps you understand what are grounding techniques and how to apply them effectively during moments of distress.
Working with a professional ensures you build a toolkit of grounding strategies that actually work for your nervous system, not just generic exercises that might feel disconnected from your experience.
When it helps most
Professional support proves most valuable when grounding techniques alone don’t stop intrusive thoughts or flashbacks. You benefit from trauma-informed therapy if anxiety interferes with daily activities, past trauma resurfaces unexpectedly, or self-guided techniques feel overwhelming. This collaborative approach works especially well when preparing for stressful situations or processing specific traumatic events through modalities like EMDR.
Tips and safer variations
Start by researching therapists who specialize in trauma recovery and anxiety management. Ask potential providers about their training in somatic approaches and grounding strategies. Schedule a consultation call to assess whether their approach feels right for you. Consider telehealth options if transportation or schedules create barriers. Remember that building this relationship takes time, and you can request modifications to techniques that feel uncomfortable or triggering during sessions.
2. Use the 5-4-3-2-1 method
The 5-4-3-2-1 method ranks among the most widely recommended grounding techniques because it works quickly and requires no special equipment. This sensory exercise redirects your attention from internal distress to external reality by engaging all five senses in a structured countdown. You can use it anywhere, making it a reliable tool when anxiety strikes unexpectedly.

What it is
This technique asks you to identify specific sensory details in your environment using a countdown format. You name five things you see, four you can touch, three you hear, two you smell, and one you taste. The structured sequence forces your brain to focus on concrete observations rather than anxious thoughts. When people ask what are grounding techniques, this method often serves as the introduction because it addresses multiple sensory channels in one exercise.
How to do it
Start by finding a comfortable position wherever you are. Look around and name five objects you see out loud or silently. Next, notice four things you can physically touch, actually reaching out to feel their texture if possible. Identify three sounds in your environment, including distant or subtle noises. Recognize two scents, even if one is simply the air around you. Finally, notice one thing you can taste, whether it’s lingering flavor or the neutral taste inside your mouth.
This sensory countdown pulls your attention away from racing thoughts and anchors it firmly in the present moment through deliberate observation.
When it helps most
This method works best during moderate anxiety or panic attacks, especially in public settings where you need a discreet intervention. You’ll find it particularly useful when intrusive thoughts loop or when you notice early signs of dissociation. The technique proves effective before stressful events like presentations or difficult conversations, giving your nervous system a concrete task that interrupts the stress response.
Tips and safer variations
Adapt the sequence if certain senses trigger discomfort. You can repeat the entire cycle multiple times, slowing your pace with each round to deepen the grounding effect. If naming items aloud feels awkward in public, mentally catalog your observations instead. Some people prefer reversing the order (1-2-3-4-5) or focusing more time on senses that feel most calming. Skip the taste component if it triggers nausea during panic, substituting an additional sound or visual observation instead.
3. Try the 3-3-3 reset
The 3-3-3 reset offers a simplified alternative when you need quick grounding but feel too overwhelmed for longer techniques. This streamlined approach reduces the cognitive load during high anxiety moments by limiting your focus to just three elements in three categories. You complete the entire exercise in under a minute, making it ideal for sudden panic or acute stress.
What it is
This technique asks you to identify three things you see, three things you hear, and three body parts you can move. The reduced number of observations compared to the 5-4-3-2-1 method makes it accessible when your concentration feels scattered. You engage sight, sound, and physical movement to create a comprehensive grounding experience without overwhelming your already taxed nervous system.
How to do it
Begin by naming three objects in your visual field, speaking them aloud or noting them silently. Next, identify three distinct sounds, whether nearby or distant. Finally, move three different body parts in succession, such as wiggling your toes, rolling your shoulders, and stretching your fingers. You can repeat the cycle if needed, selecting different items and movements each time to deepen the grounding effect.
This simplified structure works when what are grounding techniques need to be is fast, concrete, and mentally manageable during peak distress.
When it helps most
You’ll find this reset most effective during sudden panic attacks or when unexpected triggers catch you off guard. The technique works well in crowded spaces where extensive observation might feel awkward. It helps when you need immediate grounding but feel too dysregulated to remember more complex sequences or when time pressure requires a rapid intervention.
Tips and safer variations
Choose obvious objects and sounds if your concentration feels limited. You can slow down each step, pausing between categories to regulate your breathing. Skip movements that trigger pain or discomfort, substituting gentler actions instead. Some people prefer repeating one category multiple times before moving to the next, creating their own rhythm that feels more natural and sustainable during distress.
4. Do box breathing
Box breathing creates a rhythm that directly calms your autonomic nervous system through controlled breath patterns. Military personnel and first responders use this technique to maintain composure under pressure, making it one of the most reliable grounding techniques when anxiety threatens to overwhelm you. The structured counting gives your mind a concrete task while your breath regulates your physical stress response.

What it is
This breathing pattern follows a four-count square, where you inhale, hold, exhale, and hold again for equal durations. Each phase lasts the same length, creating a balanced cycle that slows your heart rate and signals safety to your nervous system. The visualization of tracing a box helps anchor your attention, combining mental focus with physiological regulation in a way that exemplifies what are grounding techniques accomplish.
How to do it
Start by inhaling through your nose for four counts, filling your lungs completely. Hold that breath for four counts, keeping your body relaxed. Exhale slowly through your mouth for four counts, emptying your lungs fully. Hold the empty breath for four counts before beginning the cycle again. Repeat for at least four complete rounds, adjusting the count length if needed to match your comfortable breath capacity.
This structured breathing pattern interrupts your stress response by giving your parasympathetic nervous system clear signals that you’re safe.
When it helps most
Box breathing works best when you notice early anxiety symptoms like increased heart rate or shallow breathing. You’ll find it particularly useful before stressful situations where you need mental clarity, during panic attacks when your breath feels uncontrollable, or when preparing for sleep after a difficult day.
Tips and safer variations
Reduce the count to three if four feels uncomfortable or causes lightheadedness. You can increase to five or six counts as your capacity grows. Skip the holds if breath retention triggers panic, focusing only on equal inhales and exhales instead. Practice daily during calm moments to build muscle memory that activates more easily during actual distress.
5. Run cool or warm water over your hands
Physical sensation provides one of the fastest routes to grounding, and running water over your hands creates an immediate sensory anchor. This technique harnesses temperature and touch to interrupt anxious thoughts and reconnect you with your body. You can access this tool wherever you find a sink, making it a practical option during work stress, social anxiety, or unexpected panic.
What it is
This grounding method uses temperature and movement of water flowing over your skin to draw your attention away from distress. The sensation of water running across your hands creates a tangible focal point that your brain must actively process, temporarily overriding the mental patterns driving your anxiety. The temperature variation adds another layer of sensory input that exemplifies what are grounding techniques accomplish through physical redirection.
How to do it
Turn on the faucet and adjust the water to a comfortable temperature, choosing cool for alertness or warm for comfort. Place your hands under the stream and focus entirely on the sensation as water flows over your palms, fingers, and wrists. Notice the temperature, pressure, and sound. Move your hands slowly, observing how the water feels on different areas. Continue for one to three minutes, breathing naturally as you maintain your attention on the physical experience.
When it helps most
You’ll find this technique most effective during acute anxiety spikes when you need immediate sensory input. It works particularly well in workplace environments where stepping away to a restroom provides privacy and practicality. The method helps when dissociation begins, nighttime anxiety interrupts sleep, or social situations trigger overwhelming stress responses.
This simple act transforms an ordinary sink into a powerful tool for nervous system regulation, offering relief when other techniques feel too complex or demanding.
Tips and safer variations
Alternate between cool and warm temperatures if one feels more grounding than the other. You can extend the practice by also wetting your face or neck for additional sensory input. Pair the technique with slow breathing to enhance its calming effect. Skip this method if temperature extremes trigger pain or discomfort, choosing a neutral lukewarm setting instead.
6. Hold a grounding object
Carrying a specific physical object provides a portable anchor you can reach for whenever anxiety strikes. This tactile grounding technique uses touch and focused attention to interrupt distress by engaging your sense of physical connection. Many people find that a familiar object offers comfort while simultaneously pulling their awareness back to the present moment.
What it is
A grounding object serves as a tangible reminder that you exist in the here and now. You select an item with specific textures, weight, or temperature that engages your sense of touch, such as a smooth stone, textured coin, or piece of fabric. This method demonstrates what are grounding techniques can be at their simplest: a concrete tool that redirects your nervous system through deliberate physical sensation.
How to do it
Choose an object small enough to carry consistently in your pocket, bag, or desk. When anxiety rises, hold the item in your hand and focus entirely on its physical properties. Notice its temperature, weight, texture, and shape. Run your fingers across its surface, exploring every detail. Continue this focused observation for one to three minutes, allowing the sensory input to anchor your attention away from anxious thoughts.
This deliberate focus on texture and temperature gives your mind a concrete task that interrupts the spiral of anxiety and reconnects you with your physical reality.
When it helps most
This technique works particularly well during social anxiety or situations where you need a discreet intervention. You’ll find it helpful when preparing for stressful events, riding in vehicles that trigger panic, or managing anticipatory anxiety before difficult conversations.
Tips and safer variations
Select multiple objects to match different needs: cooling metal for alertness, soft fabric for comfort. You can pair this technique with breathing exercises to enhance its calming effect. Rotate objects periodically if one loses its effectiveness, keeping the sensory experience fresh and engaging.
7. Plant your feet and name five facts
This technique combines physical stability with mental clarity by anchoring you through both your body and your mind. You create two layers of grounding simultaneously: one through direct contact with the floor beneath you and another through factual statements that pull you away from emotional spirals. This dual approach makes it particularly effective when anxiety distorts your perception of reality.
What it is
This grounding method uses physical pressure and cognitive focus to interrupt distress. You deliberately press your feet into the ground while speaking five objective facts about your current situation, such as your location, the date, or concrete observations about your surroundings. This practice exemplifies what are grounding techniques achieve by redirecting both physical sensation and mental attention away from anxiety toward stable, verifiable truths.
How to do it
Stand or sit with your feet flat on the floor, shoes on or off. Press your feet firmly into the surface, noticing the solid contact and support beneath you. While maintaining this pressure, state five facts out loud or silently: “I am in my office,” “Today is Tuesday,” “My desk is brown,” “I am 32 years old,” “The walls are white.” Choose simple, undeniable truths that require no interpretation or emotional processing.
This combination of physical pressure and factual statements creates a powerful anchor that grounds you through both sensation and objective reality.
When it helps most
You’ll find this technique most effective during dissociation or derealization, when your surroundings feel unreal or distant. It works well when catastrophic thinking takes over, during flashbacks that distort your sense of time and place, or when you need to prepare for difficult conversations that might trigger emotional flooding.
Tips and safer variations
Adjust foot pressure to avoid pain or discomfort if you have physical limitations. You can include facts about loved ones or pets if environmental observations feel insufficient. Pair this technique with slow breathing to enhance its effectiveness. Sit instead of stand if balance feels unstable during acute anxiety.
8. Use progressive muscle relaxation
Progressive muscle relaxation systematically releases physical tension by deliberately tensing and relaxing specific muscle groups throughout your body. This technique teaches you to recognize the difference between tension and relaxation, building awareness of how anxiety manifests physically while giving you a concrete method to release it.
What it is
This grounding method involves contracting specific muscles for several seconds before releasing them completely. You work through your body in a structured sequence, usually starting from your feet and moving upward or beginning with your hands and progressing through different muscle groups. The contrast between tension and release helps you notice where anxiety creates physical tightness and demonstrates what are grounding techniques can achieve through body-based awareness.
How to do it
Find a comfortable seated or lying position. Start with your feet by curling your toes tightly for five seconds, then releasing completely and noticing the relaxation sensation for 10 seconds. Move to your calves, thighs, abdomen, hands, arms, shoulders, and face, tensing each area briefly before letting go. Focus entirely on the physical sensations during both the tension and release phases, observing how your muscles respond to deliberate relaxation.
This deliberate cycle of tension and release teaches your body what relaxation actually feels like, creating a reference point you can return to during stress.
When it helps most
You’ll find this technique most effective when physical tension accompanies anxiety, such as tight shoulders, clenched jaw, or rigid posture. It works well before sleep when stress prevents relaxation, during chronic anxiety that creates persistent muscle tension, or after stressful events when your body remains activated.
Tips and safer variations
Skip muscle groups that cause pain or cramping when tensed. You can reduce tension time to three seconds if five feels uncomfortable or increase relaxation time to 15 seconds if you need deeper release. Practice lying down if sitting creates tension, or focus only on upper body areas if full-body practice feels overwhelming.
9. Count backward or sort by categories
Mental tasks that require focused calculation or categorization pull your attention away from anxiety by engaging your cognitive processing. This technique redirects your brain from emotional spirals to concrete mental work, creating distance from distressing thoughts while keeping you grounded in the present moment.
What it is
This grounding method uses deliberate mental challenges to interrupt anxious thought patterns. You engage your working memory by counting backward from 100 by threes or sevens, or by sorting objects in your environment into specific categories like colors, shapes, or alphabetical order. These tasks demonstrate what are grounding techniques accomplish through cognitive redirection rather than sensory focus.
How to do it
Choose a counting pattern that requires active concentration, such as 100, 97, 94, 91, continuing until you reach zero. Alternatively, scan your environment and mentally categorize items: list every blue object you see, name things in alphabetical order, or group items by shape. Speak your observations aloud or maintain them silently, depending on your setting and privacy needs.
This mental engagement forces your brain to shift from emotional processing to logical task completion, interrupting the anxiety spiral through cognitive demand.
When it helps most
You’ll find this technique most effective during racing thoughts or rumination cycles that loop without resolution. It works well when sensory grounding feels insufficient, during insomnia triggered by anxiety, or when you need discreet intervention in public spaces where physical techniques might draw attention.
Tips and safer variations
Start with easier counts like twos or fives if sevens feel overwhelming during acute distress. You can combine counting with breath patterns, such as one number per exhale. Choose categories that feel neutral and engaging rather than emotionally charged topics that might trigger additional stress.
10. Take a sensory walk
Movement combined with deliberate sensory attention creates a powerful grounding experience that engages both your body and mind. A sensory walk transforms routine movement into a focused practice that pulls you out of anxious thoughts and into direct contact with your physical environment. You can adapt this technique to any setting, from your home to outdoor spaces.

What it is
This grounding method involves walking slowly while intentionally noticing sensory details around you. Unlike regular walking where your mind wanders, you maintain focused awareness on what you see, hear, feel, and smell during movement. This practice combines the regulating effects of physical activity with the anchoring power of sensory observation, showing what are grounding techniques accomplish through integrated mind-body engagement.
How to do it
Begin walking at a slower pace than usual, paying attention to how your feet contact the ground with each step. Notice the temperature of the air on your skin, sounds in your environment, colors and shapes around you, and any scents you encounter. Mentally name observations as you walk: “I feel the breeze,” “I hear birds,” “I see a red car.” Continue for five to fifteen minutes, returning your attention to sensory details whenever your mind wanders.
This deliberate fusion of movement and sensory observation disrupts anxiety patterns while your body releases tension through physical activity.
When it helps most
You’ll find this technique most effective during moderate anxiety or restlessness when sitting still feels impossible. It works well when you need a break from overwhelming environments, during the early stages of panic before it peaks, or when you’ve been sedentary for extended periods and need physical grounding.
Tips and safer variations
Choose safe, familiar routes if spatial awareness feels compromised during distress. You can walk indoors if weather or safety concerns limit outdoor access. Reduce your pace further if balance feels unstable, or focus on fewer sensory channels if tracking multiple inputs feels overwhelming.
11. Use music or scent as an anchor
Familiar sensory experiences like specific songs or scents create powerful anchors that can instantly shift your emotional state. Your brain associates certain sounds and smells with safety or calm moments, allowing you to activate those feelings when anxiety rises. This technique harnesses your sensory memory to ground you through deliberate exposure to pre-selected anchors.
What it is
This grounding method uses intentional sensory pairing to create reliable calm triggers. You select specific music tracks or scents that evoke peace, then expose yourself to them during both calm and distressed states. Over time, these anchors become neurological shortcuts that signal safety to your nervous system. This practice shows what are grounding techniques can achieve through deliberate sensory conditioning rather than real-time observation.
This intentional pairing transforms everyday sensory experiences into reliable tools that activate calm responses when your nervous system needs regulation most.
How to do it
Choose one song or scent that feels genuinely calming rather than triggering. Practice experiencing it during peaceful moments to strengthen the association with relaxation. When anxiety strikes, activate your anchor by playing the song or inhaling the scent. Focus entirely on the sensory experience for two to five minutes, breathing naturally as you allow the familiar input to regulate your nervous system.
When it helps most
You’ll find this technique most effective during anticipated anxiety, such as before medical appointments or difficult conversations. It works well when you need discreet intervention in public settings, during travel that triggers distress, or when creating evening routines that signal your body to transition from stress to rest.
Tips and safer variations
Avoid music or scents connected to traumatic memories or triggering situations. You can create multiple anchors for different needs: energizing scents for morning anxiety, calming music for sleep preparation. Pair this technique with breathing exercises to deepen its effect.
Next steps
You now have 11 practical answers to what are grounding techniques and how to use them when anxiety strikes. These tools work best when you practice them regularly during calm moments, building the neural pathways that activate more easily during actual distress. Start with one or two methods that feel most accessible, then expand your toolkit as you discover which techniques regulate your nervous system most effectively.
Professional support amplifies the effectiveness of these grounding strategies. A trauma-informed therapist helps you understand your specific triggers, customize techniques to your needs, and process the underlying experiences that drive your anxiety. They provide the structured environment where you can practice these skills safely while addressing the root causes of your distress.
If you’re ready to build a sustainable grounding practice with professional guidance, Trellis Counseling in Oregon specializes in trauma-informed therapy that integrates these practical tools with deeper healing work. We help you develop personalized strategies that actually work for your nervous system.