Richard Schwartz Internal Family Systems: A Complete Guide
When you’re struggling with trauma, anxiety, or overwhelming emotions, finding a therapy approach that actually makes sense can feel like searching in the dark. Richard Schwartz Internal Family Systems (IFS) has emerged as one of the most effective and accessible frameworks for understanding how our minds work, and more importantly, how healing happens.
Dr. Richard Schwartz, a family therapist who stumbled onto something revolutionary while working with eating disorder patients in the 1980s, developed a model that treats the mind as a natural system of protective and wounded parts. Rather than viewing conflicting thoughts and emotions as problems to eliminate, IFS sees them as parts of you trying to help in the only ways they know how.
At Trellis Counseling, we use IFS as one of our core therapeutic approaches because it aligns with our mission: supporting trauma survivors through evidence-based, compassionate care. This guide covers everything you need to know about Richard Schwartz, the IFS model’s foundational concepts, and resources to deepen your understanding, whether you’re considering therapy, already in treatment, or simply curious about this transformative approach.
Who Richard Schwartz is and how IFS began
Dr. Richard Schwartz didn’t set out to create a new therapy model. He was a family therapist working at the Institute for Juvenile Research in Chicago during the early 1980s when his clients began describing their internal experiences in ways that challenged everything he’d learned in graduate school. Instead of dismissing these descriptions, he listened, and what he heard changed the landscape of psychotherapy.
The accidental discovery that launched IFS
Schwartz was treating patients with eating disorders and trauma when they started talking about different “parts” of themselves that seemed to have distinct voices, feelings, and roles. One part might desperately want to binge eat while another criticized relentlessly. Rather than viewing these as pathological symptoms, he began working with these parts, treating them as a natural, protective system within each person. The results surprised him. When he helped clients access what he later called their “Self” (a calm, compassionate core), those protective parts relaxed, and deep healing became possible.
“IFS grew from listening carefully to what clients were already telling us about their inner worlds.”
His background in family systems theory gave him the framework to understand these internal dynamics. Just as families develop roles and patterns to maintain balance, Schwartz realized that our internal systems do the same thing. He spent years refining richard schwartz internal family systems into a structured therapeutic approach, eventually founding the Center for Self Leadership in 2000 and training thousands of therapists worldwide. Today, IFS is recognized as an evidence-based practice for trauma, helping people understand that there’s nothing wrong with having parts, only with how those parts learned to protect you.
What Internal Family Systems therapy is
Internal Family Systems therapy is a structured approach that helps you understand and heal your internal world by working directly with the different parts of your personality. Instead of trying to eliminate difficult thoughts or emotions, IFS treats these as protective parts that developed to keep you safe during overwhelming experiences. You learn to listen to these parts with curiosity rather than judgment, uncovering why they behave the way they do and what they’re trying to protect you from.
A non-pathologizing approach to healing
Richard schwartz internal family systems fundamentally reframes what most people consider psychological symptoms. When you experience anxiety, depression, or self-sabotaging behaviors, IFS doesn’t label these as disorders that need fixing. Instead, your therapist helps you recognize these as adaptive responses from parts that are stuck in the past, still trying to protect you from dangers that may no longer exist.
“IFS assumes you already have everything you need to heal within you.”
How IFS differs from traditional therapy
Traditional therapy often focuses on managing symptoms or changing thought patterns from the outside. IFS works from the inside out, helping you access your Self (your core wisdom and compassion) to heal wounded parts directly. You’re not passive in this process. Your therapist guides you to become the primary healer of your own system, building internal relationships that last long after therapy ends.
Key concepts: parts, Self, and inner healing
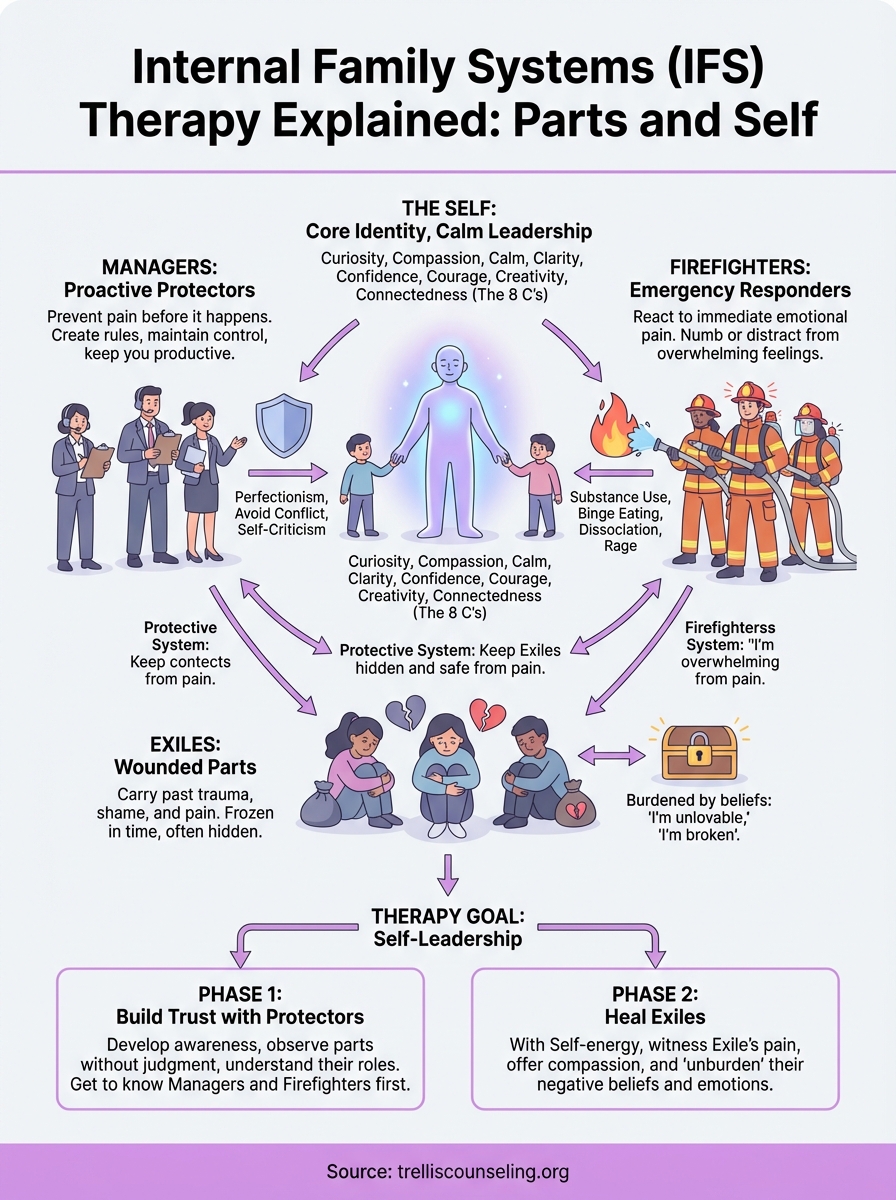
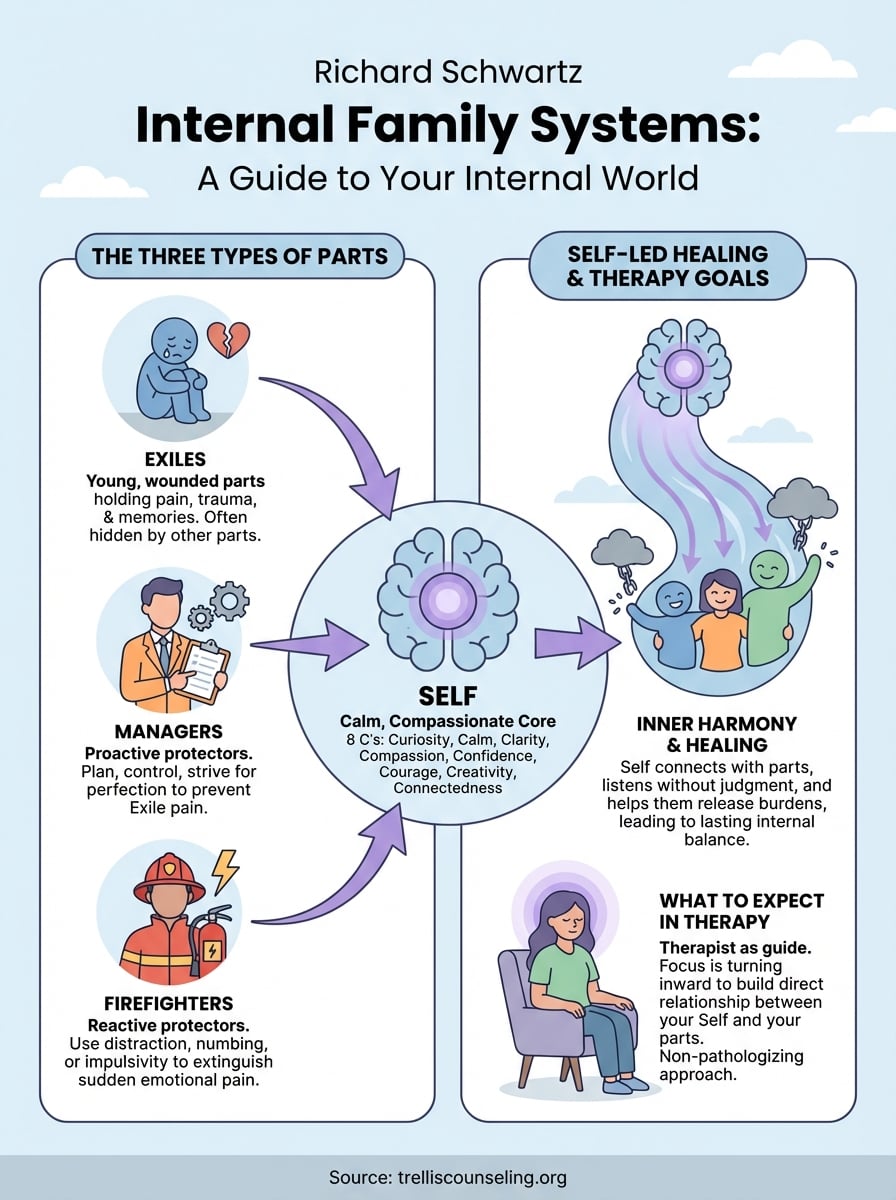
Richard schwartz internal family systems rests on three foundational concepts that make it both accessible and profoundly effective. Parts are the sub-personalities within you that developed to handle specific emotions or experiences. The Self is your innate core of calm, compassion, and wisdom that can heal these parts. Inner healing happens when your Self connects with wounded parts, helping them release the burdens they’ve been carrying since traumatic experiences.
Understanding parts and their roles
Your parts fall into three categories. Exiles are the young, wounded parts that hold painful memories and emotions from the past. Managers work proactively to keep you functioning and prevent exiles from overwhelming you through perfectionism, control, or planning. Firefighters react when exiles break through, using distraction or numbing behaviors like substance use, binge eating, or self-harm to extinguish emotional pain quickly.

“No part is inherently bad. Each developed to protect you when you needed protection most.”
How Self-led healing transforms your system
When you access your Self energy (characterized by the 8 C’s: curiosity, calm, clarity, compassion, confidence, courage, creativity, and connectedness), you become capable of healing your own parts. Your Self asks parts what they’re protecting, listens without judgment, and helps them release the extreme beliefs and emotions they’ve carried. This internal relationship becomes the foundation for lasting change, as parts learn they no longer need to use outdated strategies to keep you safe.
What to expect in IFS therapy sessions
IFS therapy sessions look different from traditional talk therapy because you spend most of your time turning inward rather than analyzing problems with your therapist. Your counselor acts as a guide and facilitator, helping you access your Self and build direct relationships with your parts. Sessions typically last 50 to 60 minutes, and while the pace varies based on what your system needs, you’ll notice a consistent structure that creates safety for vulnerable parts to emerge.
The typical IFS session structure
Your therapist begins by helping you notice what’s present in your body or mind. You might identify tension, emotions, or thoughts that signal a part wants attention. Instead of talking about this part from a distance, your counselor asks you to focus on it directly and notice what happens. They’ll check whether you’re in Self energy by asking how you feel toward the part. If you notice judgment, fear, or other reactions, those are additional parts that need acknowledgment before continuing.

“IFS therapy teaches you to become the therapist for your own internal system.”
What your therapist will guide you through
Once you’re in Self, your therapist helps you ask the part questions like what it wants you to know, what it’s afraid would happen if it stopped its role, or what it’s protecting. Richard schwartz internal family systems calls this “direct access” because you’re communicating with parts yourself rather than having your therapist interpret them. Your counselor tracks the process, ensures you stay in Self energy, and helps when parts feel stuck or overwhelmed.
Evidence, criticisms, and FAQs
Richard schwartz internal family systems has gained significant research support since its development, though like any therapeutic approach, it faces questions and criticisms worth understanding. You deserve to know what scientific evidence backs IFS and where gaps remain, as well as answers to the most common questions people ask before starting this type of therapy.
What research says about IFS effectiveness
Multiple studies demonstrate that IFS reduces symptoms of depression, anxiety, and PTSD in trauma survivors. A 2017 pilot study showed significant improvement in rheumatoid arthritis patients who used IFS for pain management. Research published in peer-reviewed journals has documented IFS effectiveness for treating eating disorders, phobias, and complex trauma. The model received approval from the National Registry of Evidence-Based Programs and Practices, validating its clinical foundation.
“While more large-scale studies are needed, existing research consistently shows positive outcomes for IFS therapy.”
Common questions and concerns
Critics point out that IFS needs more randomized controlled trials to match the research base of approaches like CBT. Some question whether the parts metaphor oversimplifies complex psychological processes. You might wonder if having parts means something is wrong with you (it doesn’t; everyone has them). Another frequent question is whether IFS works if you can’t visualize parts clearly. It does because sensing, feeling, or simply knowing about parts works equally well. Most people ask how long IFS therapy takes, and the answer varies based on your history and goals, typically ranging from several months to a few years.
Next steps if you want IFS therapy
Starting richard schwartz internal family systems therapy requires finding a trained IFS therapist who can guide you through the process of connecting with your parts and Self. You can search the official IFS therapist directory at selfleadership.org, look for practitioners who’ve completed at least Level 1 training, and schedule consultation calls to find the right fit for your needs.
Our team at Trellis Counseling includes therapists trained in IFS who work specifically with trauma survivors throughout Oregon. We offer both in-person sessions at our Milwaukee, Clackamas, and Canby locations and telehealth appointments for greater accessibility. You don’t need to wait until your symptoms become unbearable or you’ve tried everything else. The sooner you start working with your internal system, the sooner your parts can begin releasing the burdens they’ve carried for too long.