
DBT Emotional Regulation Skills: Tools For Intense Emotions
When emotions surge without warning, anger that feels uncontrollable, sadness that won’t lift, or anxiety that spirals, it can seem like your feelings have taken the driver’s seat. DBT emotional regulation skills offer a practical framework for understanding these intense experiences and responding to them more effectively. Developed as part of Dialectical Behavior Therapy, these skills give you concrete tools to work with your emotions rather than being overwhelmed by them.
At Trellis Counseling, we see firsthand how trauma and difficult life experiences can make emotional regulation feel impossible. Many of our clients in Oregon come to us struggling with emotional dysregulation tied to PTSD, anxiety, or depression. Learning DBT techniques often becomes a turning point, a way to regain stability and build resilience during recovery.
This guide walks you through the core DBT emotional regulation skills, including practical exercises and acronyms like TIPP and PLEASE that you can start using right away. Whether you’re exploring these tools on your own or alongside therapy, you’ll find strategies designed to help you manage intense emotions and move toward greater emotional balance.
Why emotional regulation skills matter in DBT
DBT emotional regulation skills form one of the four core skill modules in Dialectical Behavior Therapy, alongside mindfulness, distress tolerance, and interpersonal effectiveness. While the other modules address awareness, crisis survival, and relationships, emotional regulation focuses specifically on understanding and changing emotional experiences that cause suffering. Without these skills, many people find themselves stuck in cycles of intense reactivity, where emotions dictate behaviors that create more problems in their lives.
What happens without emotional regulation
You might notice that emotions feel like they hit out of nowhere, shift rapidly, or linger far longer than they should. This happens because your nervous system reacts to perceived threats, whether real or imagined, and triggers survival responses that made sense evolutionarily but don’t serve you well in modern life. Without regulation skills, you’re more likely to act on impulses driven by fear, anger, or shame, leading to damaged relationships, job loss, self-harm, or substance use.
When you lack tools to manage emotional intensity, your brain defaults to fight, flight, or freeze responses that often make situations worse rather than better.
People with trauma histories often experience heightened emotional sensitivity, where everyday stressors activate the same brain pathways as life-threatening events. DBT addresses this by teaching you how to recognize emotions earlier, understand what triggers them, and choose responses that align with your values rather than your immediate urges. These skills give you agency over your internal experience instead of feeling controlled by it.
The specific role in DBT treatment
DBT was originally developed for individuals with borderline personality disorder, who often struggle with intense, rapidly shifting emotions and fears of abandonment. However, therapists now use these techniques with anyone experiencing emotional dysregulation, including those with PTSD, depression, anxiety, eating disorders, or substance use issues. The skills work because they’re based on neuroscience and cognitive-behavioral principles, not just theory.
Learning emotional regulation in DBT involves both understanding the mechanics of emotions and practicing specific techniques until they become automatic. You’ll work on identifying what you’re feeling, reducing emotional vulnerability, changing unwanted emotions, and building positive experiences. This combination addresses both immediate crisis moments and long-term patterns that keep you stuck in suffering. The skills become most effective when you practice them consistently, even when you’re not in crisis, so they’re available when you need them most.
How DBT explains emotions and action urges
DBT breaks down emotions into understandable components rather than treating them as mysterious forces. Your emotional responses follow predictable patterns based on biological factors, past experiences, and current circumstances. When you understand this framework, you gain insight into why you feel what you feel and can begin using dbt emotional regulation skills more effectively. The model shows that emotions aren’t random, they arise from specific triggers and serve functions that once helped you survive.

What triggers your emotional responses
Every emotion starts with a prompting event, something that happens either externally in your environment or internally through thoughts and memories. You might see someone who reminds you of a past abuser, receive a critical email from your supervisor, or remember a traumatic experience. These events interact with your vulnerability factors, the conditions that make you more emotionally sensitive at any given moment. Poor sleep, hunger, physical pain, ongoing stress, or unresolved conflicts all increase your likelihood of having intense emotional reactions to minor triggers.
Your vulnerability factors determine whether a small inconvenience becomes a minor annoyance or triggers a full emotional crisis.
Understanding action urges vs. actions
Your emotions generate automatic urges to act in specific ways that match the feeling. Anger creates urges to attack or confront, fear produces urges to avoid or escape, and shame drives urges to hide or self-punish. These action urges are not the same as actions, and this distinction forms the foundation of emotional regulation. You can feel intense rage and experience the urge to yell without actually yelling, just as you can feel overwhelming sadness and have urges to isolate without following through.
Learning to observe the gap between urge and action gives you power over your behavior even when emotions feel completely out of control. DBT teaches you that emotions are valid information about your internal state, but the urges they create don’t have to dictate your choices. This awareness lets you pause, assess whether acting on the urge serves your long-term goals, and choose responses that align with your values rather than temporary emotional intensity.
Core DBT emotional regulation skills to practice
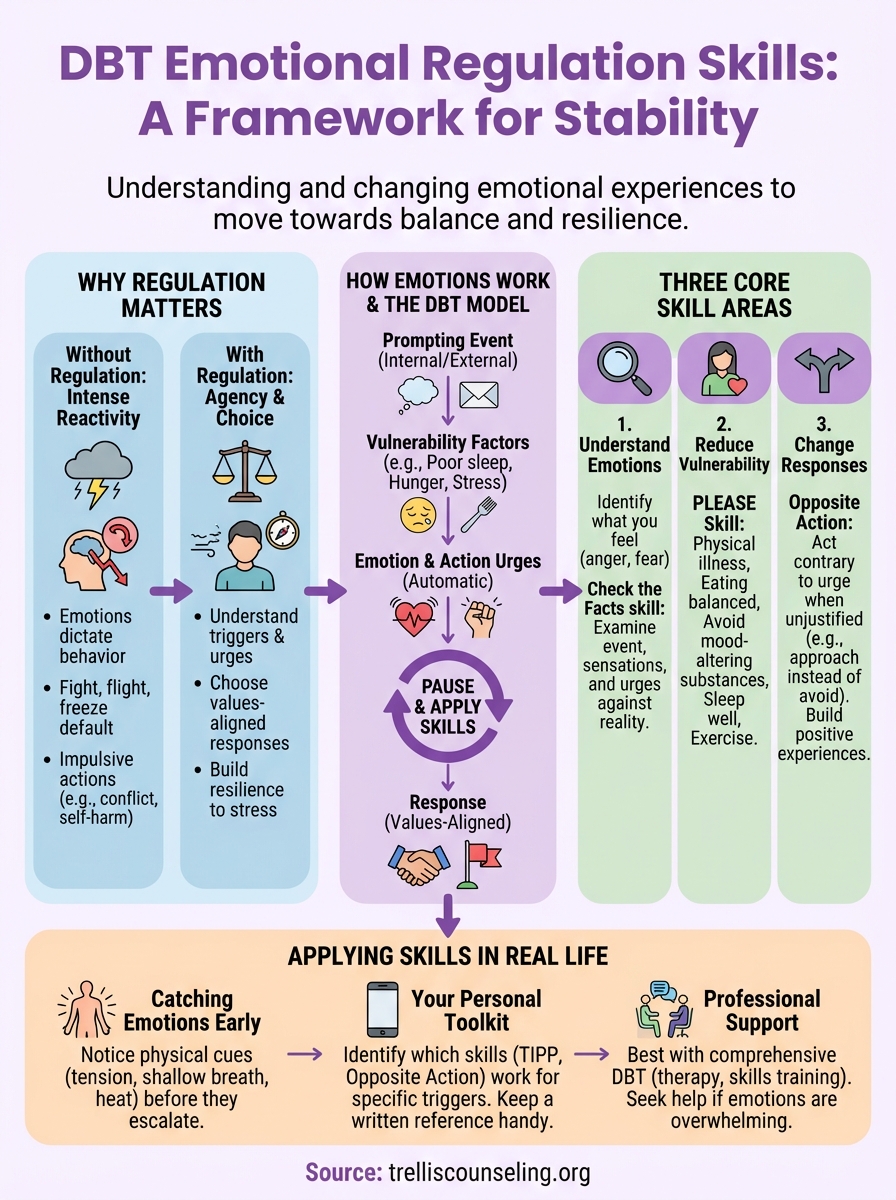
DBT organizes emotional regulation into specific, teachable skills that target different aspects of your emotional life. These techniques work together as a comprehensive system rather than isolated tools. When you practice dbt emotional regulation skills consistently, you build mental muscle memory that helps you respond more effectively when emotions intensify. The framework divides into three main skill areas, each addressing a distinct challenge in managing emotional experiences.
Understanding your current emotions
Before you can change an emotion, you need to accurately identify what you’re feeling. Many people struggle with emotional awareness, using vague terms like “bad” or “upset” instead of naming specific emotions like anger, fear, or disappointment. DBT teaches you to use the check-the-facts skill, which involves examining the prompting event, your interpretation of it, your physical sensations, action urges, and how the emotion affects your thoughts. This detailed analysis helps you determine whether your emotional intensity matches the actual threat level of the situation.
When you can name the specific emotion you’re experiencing, you gain the first tool needed to regulate it effectively.
Reducing emotional vulnerability
The PLEASE skill addresses the biological factors that make you more emotionally reactive. This acronym stands for treating Physical illness, balancing Eating, avoiding mood-altering substances, balancing Sleep, and getting Exercise. Your physical state directly impacts your emotional baseline, so neglecting these basics leaves you vulnerable to intense reactions over minor stressors. When you maintain consistent sleep schedules, eat regular meals, and move your body, you create physiological stability that supports emotional regulation.

Changing unwanted emotional responses
Opposite action involves acting contrary to your emotion-driven urges when those urges don’t match the facts or don’t serve your goals. If you feel unjustified anger, you approach gently instead of attacking. When anxiety about a safe situation drives avoidance, you move toward the feared situation instead of running away. This technique works because acting differently than your emotion suggests sends your brain new information that gradually shifts the emotional response itself.
How to use DBT skills in real-life moments
Knowing dbt emotional regulation skills doesn’t help if you can’t access them when your emotions spike. The gap between theoretical knowledge and practical application often determines whether you ride out intense feelings successfully or get swept away by them. Real-world use requires building automatic habits that kick in before your emotions reach crisis levels. You develop this capacity through consistent practice during calm moments, creating neural pathways that become accessible even when your thinking brain starts shutting down under stress.
Catching emotions early
Your body signals emotional changes before your conscious mind registers them. You might notice your jaw tightening, your breathing becoming shallow, heat rising in your chest, or tension spreading through your shoulders. These physical cues give you precious seconds to intervene before the emotion intensifies beyond easy management. When you catch yourself in these early moments, you can apply skills like opposite action or the TIPP technique to prevent escalation.
The earlier you notice an emotion building, the less intense intervention you’ll need to regulate it effectively.
Practice body scanning throughout your day, checking in with your physical state every few hours. This builds awareness that transfers to emotional situations automatically over time.
Creating your personal toolkit
Different situations require different skills, so you need to identify which techniques work best for your specific triggers. You might find that TIPP works perfectly for sudden panic but feels useless for simmering resentment, while opposite action helps with anxiety but not with grief. Create a written reference listing your most common emotional challenges and the skills that have proven effective for each one. Keep this list accessible on your phone, in your wallet, or on your bathroom mirror where you can review it when emotions cloud your memory of what actually helps.
Common questions and safety notes
You might wonder whether practicing dbt emotional regulation skills on your own carries risks or whether you’re doing the techniques correctly. These valid concerns deserve direct answers because emotional work can feel vulnerable, especially when you’re already struggling. Understanding the boundaries and limitations of self-directed practice helps you use these tools safely while recognizing when you need professional guidance.
Are these skills a replacement for therapy?
DBT skills work best when learned within a comprehensive treatment program that includes individual therapy, skills training, and phone coaching. While you can practice these techniques independently and experience real benefits, they don’t replace professional support, particularly if you have severe symptoms or trauma history. Self-practice helps reinforce what you learn in therapy but shouldn’t substitute for it if you’re experiencing suicidal thoughts, self-harm urges, substance dependence, or symptoms that interfere with daily functioning.
Working with a trained DBT therapist ensures you receive guidance tailored to your specific situation and safety needs.
What if practicing skills makes emotions worse?
Some people notice that emotional awareness initially intensifies feelings as you start paying attention to experiences you previously avoided or numbed. This temporary increase usually means you’re engaging with the work authentically rather than doing something wrong. However, if you consistently feel overwhelmed or destabilized by practicing skills, or if intense emotions persist for days without relief, you need professional evaluation. Your nervous system might require trauma-focused treatment before you can effectively use regulation techniques, or you might need medication support alongside skills training.
When you want extra support
Learning dbt emotional regulation skills on your own provides valuable tools, but many people reach a point where they need professional guidance to make lasting progress. Working with a therapist trained in DBT gives you personalized feedback on your technique, helps you navigate obstacles that feel insurmountable alone, and provides the accountability that keeps you practicing consistently. If you notice that your emotional intensity continues interfering with relationships, work, or daily functioning despite your best efforts, that’s a clear sign therapy would help.
At Trellis Counseling, our Oregon-based therapists specialize in trauma-informed approaches that include DBT skills training alongside EMDR and Internal Family Systems therapy. We understand how trauma complicates emotional regulation and create treatment plans that address your specific needs, whether you prefer in-person sessions at our Milwaukee, Clackamas, or Canby locations or virtual appointments. Contact our team to explore how professional support can help you build the emotional stability you’re working toward.






