
Cognitive Behavioral Therapy for Depression: How It Works
Cognitive Behavioral Therapy for Depression: How It Works
Depression changes how you think. It convinces you that you’re worthless, that nothing will improve, that you’re stuck. Cognitive behavioral therapy for depression works by targeting those exact thought patterns, the ones that keep you trapped in a cycle of low mood and hopelessness. It’s one of the most researched and effective treatments available, and understanding how it works can help you decide if it’s right for you.
This article breaks down the science behind CBT, the specific techniques therapists use, and what you can realistically expect from the process. Whether you’re considering therapy for the first time or exploring a different approach, you’ll find clear answers about how CBT addresses depression at its roots, not just the symptoms, but the underlying thinking patterns that fuel them.
At Trellis Counseling, we provide evidence-based treatments to help Oregonians work through depression, anxiety, and trauma. Our approach focuses on building lasting skills that change how you relate to your own thoughts and experiences. What follows is a comprehensive look at CBT so you can understand exactly what this treatment involves and whether it might support your path toward feeling like yourself again.
What CBT targets in depression
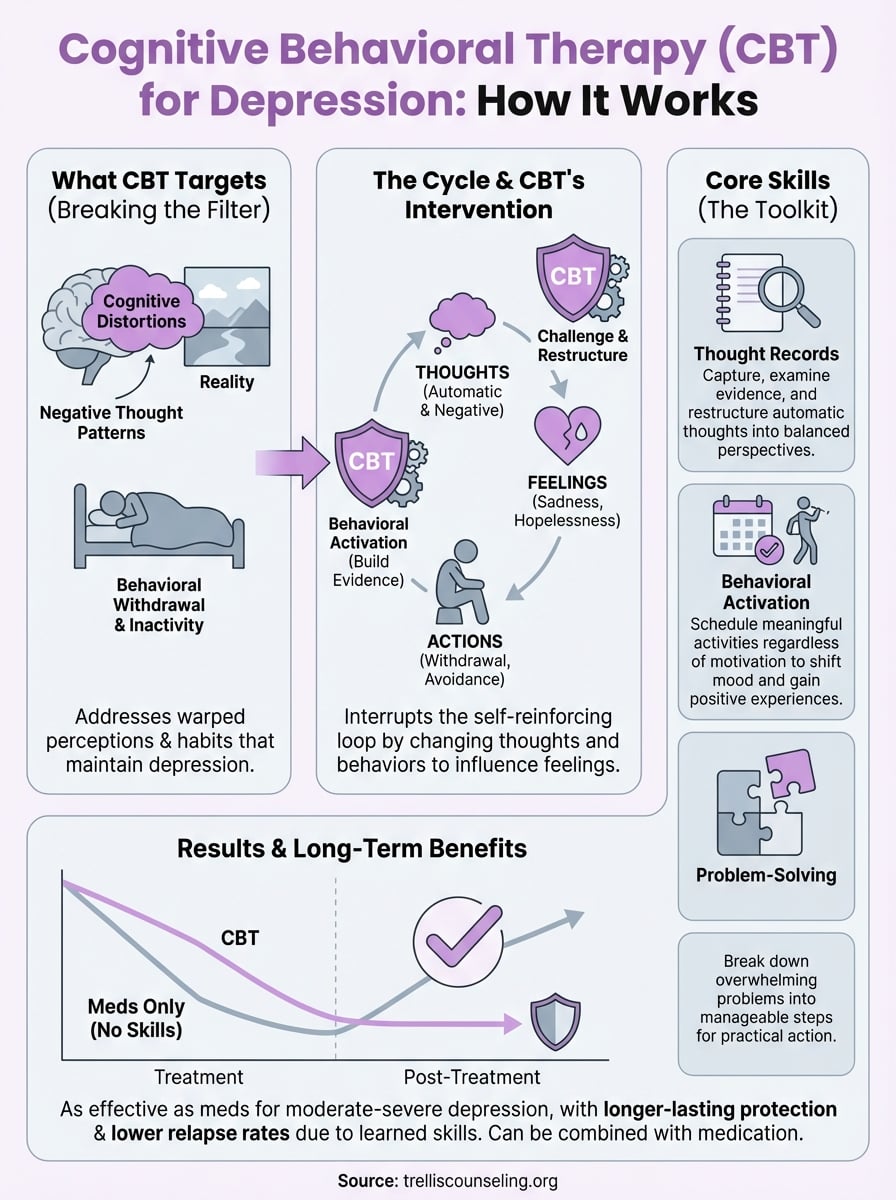
Depression doesn’t just affect your mood. It warps your entire perception of reality, creating a filter through which every experience gets interpreted negatively. Cognitive behavioral therapy for depression targets three specific areas: the negative thought patterns that fuel depressive symptoms, the behaviors that keep you stuck, and the complex relationship between how you think, feel, and act. This approach recognizes that depression isn’t just a chemical imbalance but a pattern you can learn to interrupt.
The therapy focuses on identifying and changing the automatic thoughts that pop into your head throughout the day. These thoughts often feel completely true in the moment, even when they’re distorted or irrational. CBT helps you recognize these patterns so you can challenge them rather than accepting them as facts. What makes this approach different from simply "thinking positive" is that it teaches you to examine the evidence for and against your thoughts, creating a more balanced and realistic perspective.
Negative thought patterns and cognitive distortions
Your brain develops shortcuts to process information quickly, but when you’re depressed, these shortcuts become systematic errors in thinking. Therapists call these cognitive distortions, and they include patterns like all-or-nothing thinking (seeing everything as either perfect or completely failed), overgeneralization (viewing one negative event as proof of an endless pattern), and mental filtering (focusing only on negatives while ignoring positives). You might catastrophize, jumping to the worst possible conclusion, or engage in mind reading, assuming you know what others think about you without evidence.
These distortions reinforce themselves. When you believe "I always fail," you interpret neutral or even positive events through that lens. A small mistake becomes proof of your incompetence. A friend’s distracted response becomes evidence that everyone finds you annoying. CBT trains you to spot these patterns in real time and question their accuracy before they spiral into deeper depression.
Recognizing cognitive distortions doesn’t make them disappear overnight, but it breaks their automatic power over your mood and behavior.
Behavioral patterns that maintain depression
Depression also targets what you do, or more accurately, what you stop doing. When you feel hopeless and exhausted, you naturally withdraw from activities that used to bring satisfaction or connection. You skip social events, abandon hobbies, stay in bed longer, and avoid challenges. These behaviors make perfect sense as a way to cope with feeling terrible, but they actually strengthen the depression by cutting you off from potential sources of joy and accomplishment.
CBT addresses this through behavioral activation, which involves systematically re-engaging with meaningful activities even when you don’t feel motivated. The approach recognizes that in depression, behavior often needs to change before mood improves. You don’t wait until you feel better to start doing things. Instead, you schedule specific activities and follow through regardless of how you feel, creating opportunities for positive experiences that can gradually shift your emotional state.
The relationship between thoughts, feelings, and actions
The core principle underlying CBT is that thoughts, emotions, and behaviors constantly influence each other in a continuous loop. You don’t have direct control over your feelings, but you can change how you think about situations and how you respond behaviorally. These changes then affect your emotional experience. When you believe "nothing I do matters," you feel hopeless, which leads to inaction, which produces no positive results, which reinforces the original belief.

CBT interrupts this cycle at multiple points. By changing your thoughts (challenging the belief that nothing matters), you create space for different feelings (perhaps tentative hope or curiosity). By changing your behavior (taking small actions even while feeling hopeless), you generate evidence that contradicts your negative predictions. This bidirectional approach gives you more points of intervention, making it easier to break free from depression’s self-reinforcing patterns.
What research says about CBT results
Research on cognitive behavioral therapy for depression consistently shows that it works as well as antidepressant medication for moderate to severe depression, and it provides benefits that last longer after treatment ends. Multiple large-scale studies have tracked thousands of patients through CBT programs, measuring not just immediate symptom relief but also long-term recovery rates. The evidence base is strong enough that major medical organizations recommend CBT as a first-line treatment, meaning it should be one of the first options your doctor considers, not a last resort after everything else fails.
Effectiveness compared to other treatments
CBT produces measurable improvement in roughly 50-75% of people who complete a full course of treatment, depending on how severely depressed they were at the start. When researchers compare it directly to antidepressants, the two approaches show similar effectiveness for treating active depression. Studies that followed patients after treatment ended, however, revealed a crucial difference. People who received CBT were significantly less likely to relapse into depression compared to those who only took medication and then stopped. The skills you learn in CBT continue protecting you even when therapy ends, while medication typically only works while you’re taking it.
Comparisons with other therapy types show varying results depending on what you’re measuring. Some research suggests that interpersonal therapy and behavioral activation produce similar outcomes to traditional CBT. What matters more than the specific type of therapy is whether you engage consistently with the process and practice the techniques you learn between sessions.
CBT’s advantage isn’t that it works faster than medication, but that it teaches you skills that continue working long after your last therapy session.
Long-term outcomes and relapse prevention
Follow-up studies tracking patients for one to two years after completing CBT show relapse rates around 30%, compared to 60-70% for people who stopped taking antidepressants without any therapy. This protection appears to strengthen the longer you practice CBT skills. Research indicates that people who continue using cognitive restructuring techniques and behavioral strategies report fewer depressive episodes and less severe symptoms when difficulties arise.

The long-term benefits extend beyond just preventing full relapse. Studies measuring quality of life, work functioning, and relationship satisfaction found that CBT produces sustained improvements in these areas even when people experience temporary mood dips. You develop a different relationship with negative thoughts, recognizing them as mental events rather than absolute truths, which reduces their power to trigger prolonged depressive episodes.
How CBT works in therapy sessions
Cognitive behavioral therapy for depression follows a structured, time-limited format that typically runs 12 to 20 weekly sessions, though some people need fewer or more depending on their symptoms. Each session lasts about 50 minutes and focuses on specific problems you’re experiencing right now rather than spending years exploring your childhood. The therapist acts more like a coach or teacher than a traditional analyst, actively working with you to identify thought patterns and test out new behaviors.
What happens in your first session
Your initial CBT session focuses on assessment and goal-setting. The therapist asks detailed questions about your depression symptoms, how long you’ve experienced them, what situations trigger them, and how they affect your daily life. You discuss what you want to achieve through therapy, setting concrete, measurable goals like "attend social events twice per week" or "reduce negative self-talk" rather than vague aims like "feel better." This collaborative process establishes a clear direction for your work together.
The therapist also introduces the CBT model, explaining how thoughts, feelings, and behaviors connect. You might work through a recent situation together, mapping out the thoughts that ran through your mind, the emotions you felt, and how you responded. This demonstration shows you what to expect in future sessions and starts building your ability to analyze your own experiences using this framework.
The structure of a typical CBT session
Each session follows a predictable pattern that helps you make steady progress. You start by checking in on your mood and reviewing any homework from the previous week. The middle portion tackles a specific problem or thought pattern, using techniques like thought records or behavioral experiments. You and your therapist work together to identify distortions, challenge unhelpful beliefs, and develop alternative ways of thinking or acting.
Sessions end with planning concrete homework assignments that let you practice what you learned. Your therapist might ask you to track your thoughts in specific situations, schedule pleasant activities, or try a new behavior that tests a negative belief. This structure keeps therapy focused and productive rather than wandering into unproductive territory.
The homework you complete between sessions matters as much as what happens during appointments, because that’s where you actually apply new skills to your real life.
Practice between sessions matters most
CBT requires active participation outside the therapy room. The skills you learn only become automatic through repeated practice in actual situations. Most therapists assign written exercises, asking you to complete thought records that document triggering situations, your automatic thoughts, the emotions you experienced, and alternative interpretations you can develop. Some people resist homework, viewing it as extra burden when they’re already struggling, but consistent practice directly correlates with better outcomes and faster improvement.
Core CBT skills and techniques
Cognitive behavioral therapy for depression teaches you specific, practical skills you can use whenever negative thoughts or low motivation threaten to pull you under. These techniques aren’t abstract concepts or vague advice about positive thinking. They’re concrete tools that change how you process experiences and respond to challenges. Your therapist will introduce these skills gradually, starting with the basics and building toward more advanced applications as you gain confidence.
Thought records and cognitive restructuring
Thought records form the foundation of CBT practice. You document situations that trigger negative emotions, the automatic thoughts that arise, the intensity of your feelings, and then work through evidence for and against those thoughts. This process transforms vague emotional reactions into analyzable data you can examine objectively. A typical thought record might capture your belief "I’m a failure" after making a mistake at work, then systematically list your accomplishments, the context of the error, and how you’d view the same situation if a friend experienced it.

The restructuring phase involves developing balanced alternative thoughts based on evidence rather than emotion. You’re not replacing negative thoughts with fake positivity. Instead, you identify more accurate interpretations that account for complexity and nuance rather than absolutes. When you catch yourself thinking "everyone hates me," you learn to question that generalization and develop a more realistic assessment like "some people respond positively to me, others seem neutral, and I don’t actually have evidence about what most people think."
Learning to catch and restructure automatic thoughts takes weeks of consistent practice, but the skill becomes more natural each time you use it.
Behavioral activation strategies
Behavioral activation counters the withdrawal and inactivity that depression creates. You work with your therapist to identify activities that historically brought satisfaction, meaning, or accomplishment, then schedule them into your week regardless of motivation levels. The activities range from basic self-care tasks like showering or preparing meals to social engagements, hobbies, exercise, or work projects. You rate each activity’s impact on your mood, building evidence about what actually helps versus what you assume will help.
Problem-solving skills
Depression often stems from or worsens with unsolved life problems that feel overwhelming. CBT teaches a structured approach: define the problem specifically, brainstorm multiple potential solutions without judging them, evaluate each option’s pros and cons, choose one to implement, and assess the results. This method breaks paralysis by transforming massive, unsolvable feelings into manageable steps. You learn that even imperfect action produces better outcomes than avoiding problems until they grow larger.
CBT and antidepressants: choosing the right mix
Many people facing depression wonder whether they should pursue cognitive behavioral therapy for depression, medication, or both at the same time. The answer depends on several factors including the severity of your symptoms, your personal preferences, past treatment responses, and what resources you can access. Research shows that both approaches work independently, and combining them can produce stronger initial results for some people, though the long-term outcomes look similar whether you use medication, therapy, or both together.
When to combine treatments
Combining CBT with antidepressants makes sense when your depression symptoms are severe enough that they interfere with your ability to engage in therapy. If you struggle to concentrate during sessions, can’t complete homework assignments, or feel too exhausted to practice new skills, medication can provide the initial stability you need to participate fully in CBT. Studies show that people with severe depression often respond better to combination treatment than to either approach alone, at least in the first few months.
You might also consider both treatments if you’ve tried therapy or medication alone without sufficient improvement. Adding the second approach gives your brain different pathways to recovery. Some people find that medication lifts their mood enough to make therapy more effective, while others discover that therapy skills help them reduce or eventually eliminate medication under their doctor’s supervision.
Combination treatment isn’t always better, but it provides two different mechanisms working on your depression simultaneously.
Starting with one approach first
Research supports starting with CBT alone if you have mild to moderate depression and can access quality therapy. This approach avoids potential medication side effects and builds skills that continue protecting you after treatment ends. The catch is that therapy requires more active effort and time commitment than taking a pill, and you need to find a trained CBT therapist, which isn’t always easy depending on where you live.
Starting with medication makes sense if you need faster symptom relief, can’t access therapy immediately, or have physical symptoms like severe insomnia or appetite changes that need medical attention. Antidepressants typically start working within two to six weeks, while CBT often takes longer to show full effects.
Adjusting your treatment plan over time
Your initial choice doesn’t lock you into a permanent path. Many people start with medication for quick stabilization, then add therapy to build lasting skills. Others begin with CBT and add medication if they’re not improving fast enough. You can also taper off medication once you’ve developed strong CBT skills, though this decision should always involve your prescriber’s guidance and careful monitoring of your symptoms.
When CBT may not be enough
Cognitive behavioral therapy for depression works for many people, but not everyone responds equally well to this approach. Some individuals need additional interventions, different therapeutic modalities, or more intensive support to manage their symptoms. Recognizing when CBT isn’t providing sufficient relief helps you adjust your treatment plan before spending months on an approach that won’t meet your needs.
Complex trauma and severe symptoms
CBT’s structured, present-focused approach sometimes struggles to address deep trauma or symptoms that extend beyond negative thought patterns. If you experienced childhood abuse, complex post-traumatic stress, or multiple traumatic events, you might need trauma-specific therapies like EMDR (Eye Movement Desensitization and Reprocessing) or trauma-focused cognitive behavioral therapy before standard CBT can help with depression. Your depression may stem from unprocessed traumatic memories that require specialized treatment to access and resolve.
Severe depression with psychotic features, intense suicidal ideation, or significant impairment in basic functioning often requires more intensive intervention than weekly outpatient CBT provides. You might need hospitalization, partial hospitalization programs, or intensive outpatient treatment that offers multiple therapy sessions per week plus medication management. Standard CBT works best when you can engage with the material and complete homework, which becomes difficult when depression reaches severe levels.
CBT provides powerful tools for many people with depression, but it’s one approach among many, not a universal solution.
Signs you need to explore other options
You should consider additional or alternative treatments if you’ve completed 8 to 12 sessions of CBT without noticeable improvement in your mood or functioning. While therapy often takes time, you should see at least small positive changes within the first few months. Persistent symptoms despite consistent homework completion and active participation suggest that CBT alone may not address your particular depression.
Other warning signs include worsening symptoms during treatment, difficulty understanding or applying CBT concepts despite repeated explanations, or discovering that your depression stems from ongoing life circumstances that require practical solutions rather than cognitive restructuring. You might also need different support if you have co-occurring conditions like bipolar disorder, severe anxiety disorders, or substance use issues that interfere with CBT’s effectiveness. These situations don’t mean you failed at therapy; they mean your depression requires a different or more comprehensive treatment approach.
What to do next
Cognitive behavioral therapy for depression provides proven tools to change the thought patterns and behaviors that keep you stuck in hopelessness. The research shows clear benefits, the techniques are specific and learnable, and the skills continue protecting you long after therapy ends. Understanding how CBT works helps you make informed decisions about your treatment, but reading about it differs from actually practicing these skills with a trained therapist who can guide you through the challenging moments.
If you’re experiencing depression, taking the first step toward treatment matters more than finding the perfect approach immediately. Start by talking with your doctor or reaching out to therapists who specialize in evidence-based treatments for depression. Many people benefit from combining professional support with structured practice, while others need medication alongside therapy to manage their symptoms effectively during the recovery process.
Trellis Counseling offers trauma-informed therapy for Oregonians dealing with depression, anxiety, and related challenges. Our therapists use evidence-based approaches like CBT to help you build skills that create lasting change, not just temporary relief from your current symptoms.
