Therapy For Depression And Anxiety: 12 Effective Approaches
Depression and anxiety often show up together, creating a cycle that can feel impossible to break on your own. You might notice the weight of sadness pulling you down while racing thoughts keep you up at night. The good news is that therapy for depression and anxiety offers real, evidence-based paths forward, and there’s more than one way to get there. Finding the right approach matters because what works for one person may not work for another.
At Trellis Counseling, we’ve seen firsthand how different therapeutic methods can help people reclaim their lives. Some clients respond well to structured, goal-oriented techniques, while others benefit from exploring deeper emotional patterns. Understanding your options puts you in the driver’s seat of your own recovery. It also helps you have more productive conversations with therapists about what might fit your specific situation.
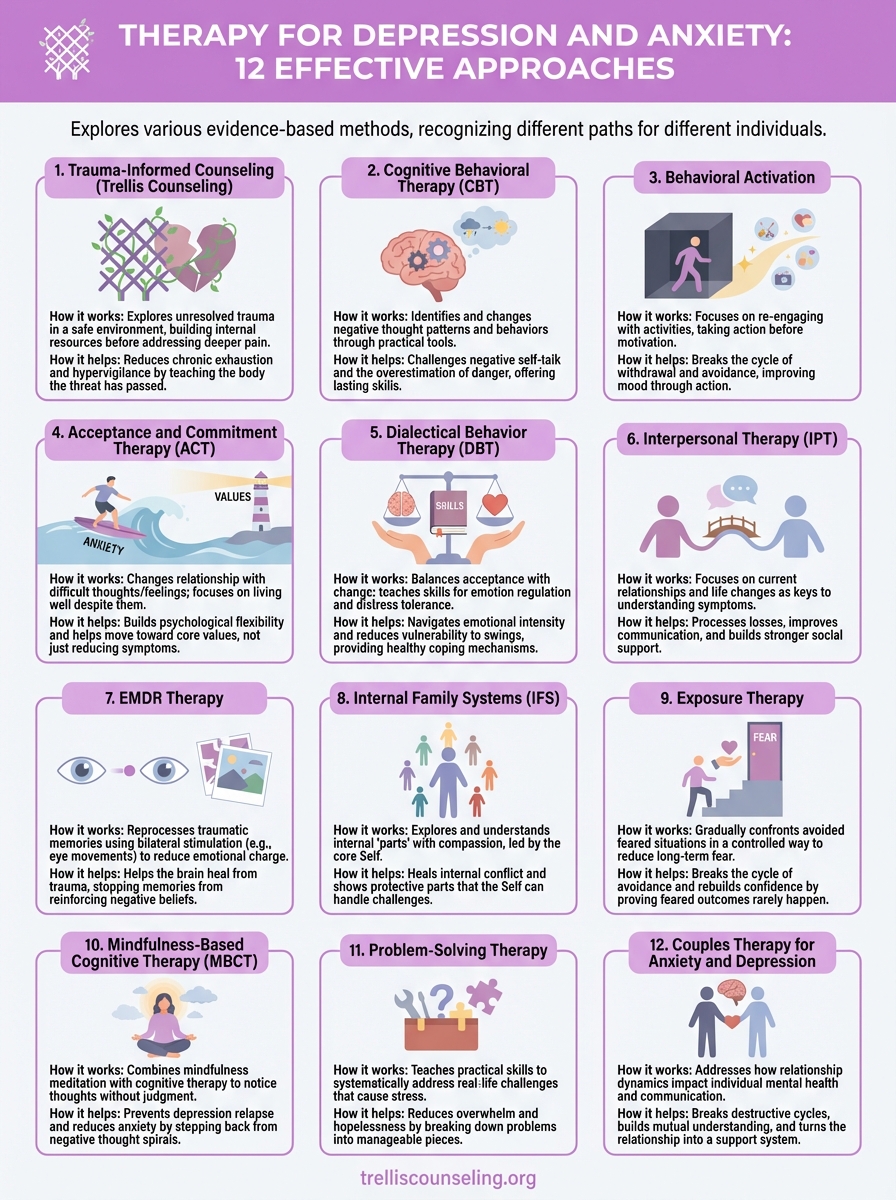
This guide breaks down 12 effective therapy approaches used to treat depression and anxiety. You’ll learn how each method works, what to expect during sessions, and who tends to benefit most from each approach. Whether you’re considering therapy for the first time or looking to try something different, this information will help you make an informed choice. Let’s walk through the options so you can take the next step toward feeling like yourself again.
1. Trauma-informed counseling at Trellis Counseling
Trauma-informed counseling recognizes how past traumatic experiences shape your current mental health challenges. At Trellis Counseling, therapists understand that depression and anxiety often stem from unresolved trauma, whether you remember specific events or simply feel their lingering effects. This approach creates a foundation of safety and trust, allowing you to explore difficult emotions without feeling retraumatized. The name “Trellis” reflects how support structures help you grow around past pain rather than trying to erase it.
How it works
Trauma-informed therapy for depression and anxiety starts with establishing physical and emotional safety in the therapeutic relationship. Your therapist at Trellis Counseling will work at your pace, never pushing you to discuss details before you’re ready. The approach uses specialized modalities like Eye Movement Desensitization and Reprocessing (EMDR) and Internal Family Systems (IFS) to process traumatic memories that fuel your current symptoms. Therapists focus on building your internal resources first, teaching you grounding techniques and emotional regulation skills. This foundation makes it possible to address deeper trauma without becoming overwhelmed.
How it helps depression and anxiety
Depression often develops when your nervous system remains stuck in protective shutdown mode after trauma. Trauma-informed counseling helps your body recognize that the threat has passed, reducing the chronic exhaustion and hopelessness you feel. For anxiety, this approach addresses the hypervigilance and constant worry that stem from past experiences when your safety was genuinely at risk. Your therapist helps you distinguish between real present-day concerns and anxiety triggered by old memories. Many clients find that addressing the root trauma provides more lasting relief than only treating surface symptoms.
“When you understand how trauma rewired your nervous system, you can begin to rewire it again toward healing.”
Who it is for
This approach works well if you’ve experienced specific traumatic events like domestic violence, accidents, assault, or combat. You don’t need to have a PTSD diagnosis to benefit from trauma-informed care. The method also helps if you’ve lived through ongoing adverse experiences such as childhood neglect, bullying, or unstable home environments. Teenagers and adults who feel like traditional talk therapy hasn’t worked often respond better when therapists address the underlying trauma. If you notice that certain situations trigger intense emotional reactions that seem out of proportion, trauma-informed counseling can help you understand why.
What to expect from sessions
Your first sessions focus on building rapport and helping you feel safe in the therapeutic space. Therapists at Trellis Counseling will ask about your current symptoms and goals without requiring you to recount traumatic details right away. Sessions typically last 50 to 60 minutes and follow a pace you help determine. Your therapist might teach you breathing exercises or grounding techniques early on, giving you tools to use between sessions. As therapy progresses, you’ll work through difficult material in manageable doses, with regular check-ins about how you’re handling the process.
Cost and access
Trellis Counseling operates physical locations in Milwaukee, Clackamas, and Canby, Oregon, plus offers telehealth services for Oregon residents who need remote access. Session costs vary based on your therapist’s credentials and whether you use insurance or pay out of pocket. The practice accepts multiple insurance plans, and staff can verify your coverage before you start. You can request appointments through their online administrative system, which also lets you manage records and communicate with your therapist. If you’re ready to explore trauma-informed counseling, reaching out to Trellis Counseling gives you access to therapists who specialize in helping survivors rebuild their lives.
2. Cognitive behavioral therapy
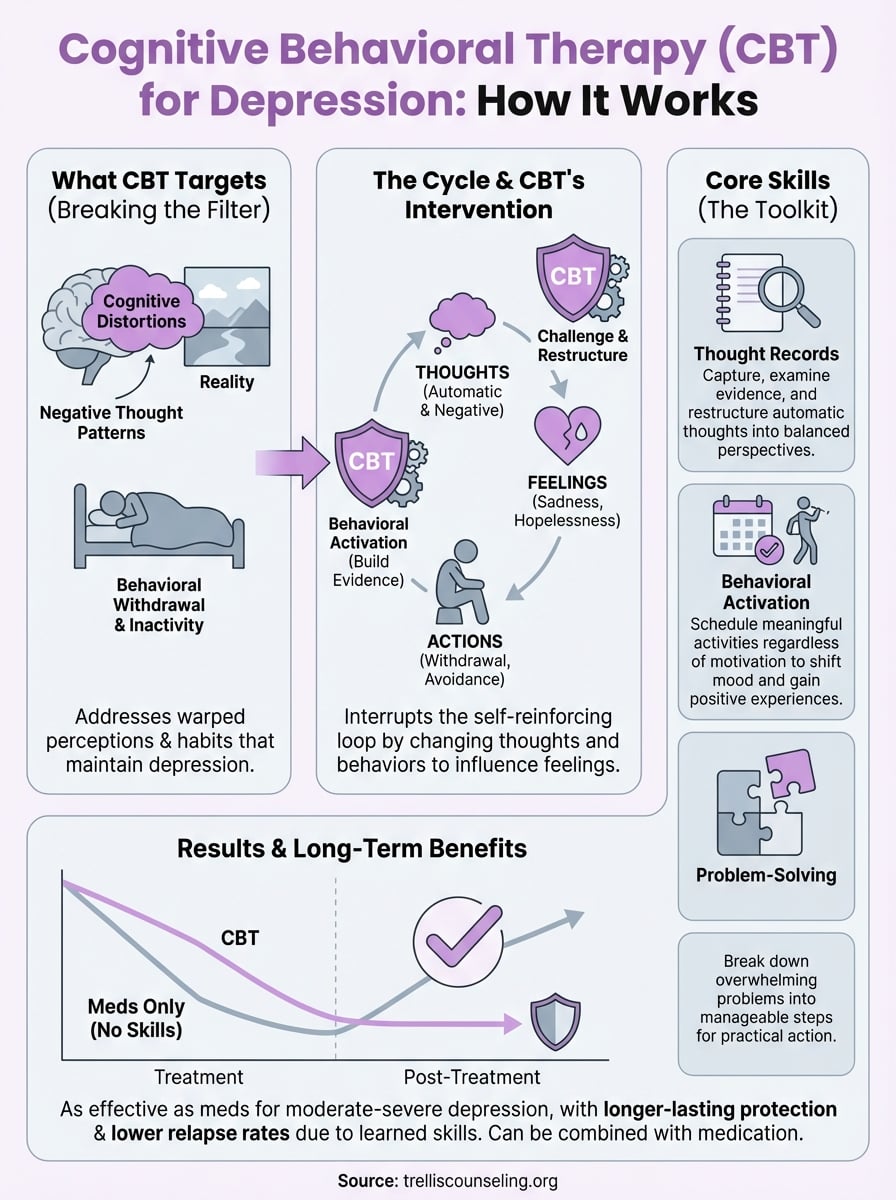
Cognitive behavioral therapy (CBT) stands as one of the most researched and widely used treatments for depression and anxiety. This approach focuses on the connection between your thoughts, feelings, and behaviors, helping you identify and change patterns that keep you stuck. Unlike therapies that explore your past for years, CBT gives you practical tools you can use right away. The method works on the principle that changing how you think about situations can change how you feel and act in response to them.

How it works
CBT operates on the idea that your automatic thoughts create emotional reactions and behavioral responses. Your therapist helps you notice negative thought patterns that distort your perception of reality, such as catastrophizing or all-or-nothing thinking. You’ll learn to examine evidence for and against these thoughts, then develop more balanced perspectives. The therapy includes homework assignments where you practice new thinking patterns and behaviors between sessions. Your therapist might ask you to keep thought records that track situations, your automatic thoughts, emotions, and alternative responses.
How it helps depression and anxiety
For depression, CBT addresses the negative self-talk and hopeless thinking that fuel low mood and withdrawal from activities. You’ll challenge beliefs like “I’m worthless” or “Nothing will ever get better” by examining concrete evidence from your life. With anxiety, CBT targets the overestimation of danger and underestimation of your ability to cope. Your therapist helps you test feared predictions through behavioral experiments, showing you that catastrophic outcomes rarely happen. Research shows CBT creates lasting changes because you learn skills you can use independently after therapy ends.
“When you change the lens through which you view your life, the picture itself transforms.”
Who it is for
CBT works well if you want structured, goal-oriented therapy with clear milestones and homework between sessions. This therapy for depression and anxiety suits people who prefer logical problem-solving over emotional exploration. You’ll benefit most if you’re willing to actively participate, complete assignments, and practice new skills regularly. The approach helps those with specific anxiety disorders like social anxiety, panic disorder, or generalized anxiety disorder. CBT also works for depression ranging from mild to moderate severity, though severe depression may require medication alongside therapy.
What to expect from sessions
Sessions typically last 50 minutes and follow a structured format with an agenda you help create. Your therapist starts by reviewing your homework and current mood, then focuses on specific problems you’re facing. You’ll spend time identifying thought patterns and developing alternative perspectives together. Each session ends with new homework assignments designed to practice skills in real-world situations. Most people attend weekly sessions for 12 to 20 weeks, though your timeline depends on your specific needs and progress.
Cost and access
CBT therapists work in private practices, community mental health centers, and hospitals across the country. Many insurance plans cover CBT when provided by licensed mental health professionals like psychologists, licensed clinical social workers, or licensed professional counselors. Session costs range from $100 to $250 without insurance, though community centers often offer sliding scale fees. You can find CBT therapists through Psychology Today’s directory or by asking your primary care doctor for referrals. Some therapists now offer telehealth CBT sessions, expanding access for people in rural areas or with transportation challenges.
3. Behavioral activation
Behavioral activation takes a different approach from traditional talk therapy by focusing on what you do rather than just what you think. This therapy for depression and anxiety works on the principle that your actions directly influence your mood, not the other way around. When you’re depressed, you naturally withdraw from activities, which then deepens your depression in a downward spiral. Behavioral activation breaks this cycle by helping you re-engage with life through purposeful action, even when you don’t feel like it.
How it works
Your therapist helps you identify activities that once brought satisfaction or aligned with your values, then creates a schedule to reintroduce them into your life. You start with small, manageable steps rather than overwhelming yourself with major changes. The therapy tracks how different activities affect your mood through daily monitoring forms that reveal patterns between what you do and how you feel. Behavioral activation doesn’t require you to change your thoughts first. Instead, you take action and let improved mood follow naturally from increased engagement with meaningful activities.
How it helps depression and anxiety
Depression thrives on inactivity and isolation, which behavioral activation directly challenges. When you engage in activities, even simple ones like walking outside or calling a friend, you interrupt the withdrawal pattern that maintains depression. For anxiety, this approach reduces avoidance behaviors that give temporary relief but worsen fear long-term. You build confidence by facing situations you’ve been dodging, proving to yourself that you can handle more than anxiety tells you. Research shows behavioral activation works as well as antidepressants for moderate depression, and the benefits continue after therapy ends.
“Action precedes motivation. You don’t wait to feel better before living your life; you live your life and feel better as a result.”
Who it is for
This approach suits you if overthinking and rumination dominate your experience of depression. Behavioral activation works particularly well when you’ve withdrawn from activities that once mattered to you, whether hobbies, relationships, or responsibilities. You’ll benefit if you prefer concrete action steps over exploring childhood experiences or deep emotional processing. The method helps people who feel stuck in inertia, knowing what they should do but struggling to start. Behavioral activation also works for anxiety when avoidance patterns have narrowed your life significantly.
What to expect from sessions
Sessions focus on reviewing your activity logs and planning the week ahead together. Your therapist helps you identify obstacles that prevented planned activities and problem-solve solutions for next time. You’ll discuss how activities affected your mood and adjust your schedule based on what works. Homework forms the core of this therapy, with daily tracking and scheduled activities between sessions. Most people attend 8 to 16 weekly sessions, though some notice mood improvements within the first few weeks.
Cost and access
Behavioral activation therapists work in community mental health centers, private practices, and hospital systems throughout the country. Many psychologists and clinical social workers incorporate behavioral activation into their treatment approach. Session costs typically range from $80 to $200 depending on location and provider credentials. Insurance coverage mirrors standard outpatient therapy benefits, though you should verify your specific plan. Some therapists offer telehealth sessions, making this treatment accessible regardless of your location or transportation situation.
4. Acceptance and commitment therapy
Acceptance and commitment therapy (ACT) takes a fundamentally different approach to treating depression and anxiety by teaching you to change your relationship with difficult thoughts and feelings rather than trying to eliminate them. This therapy for depression and anxiety recognizes that pain is part of life, and the struggle to avoid or control uncomfortable emotions often creates more suffering than the emotions themselves. ACT helps you build psychological flexibility, allowing you to move toward what matters most even when anxiety or depression shows up along the way.

How it works
ACT uses six core processes to build psychological flexibility: acceptance, cognitive defusion, being present, self-as-context, values clarification, and committed action. Your therapist teaches you to notice thoughts without believing them or fighting them, creating distance between you and your mental content. Instead of asking “How can I stop feeling anxious?” you learn to ask “How can I live well even with this anxiety?” Metaphors and experiential exercises help you practice these skills during sessions. You’ll identify your core values and take concrete steps toward them, regardless of what your mind says about your limitations.
How it helps depression and anxiety
Depression convinces you that feeling bad means you can’t do meaningful things, but ACT breaks this connection by teaching you to act on values despite mood. You stop waiting for depression to lift before living your life. For anxiety, ACT reduces the secondary suffering that comes from fighting or fearing your anxious thoughts. You learn that having the thought “I might fail” doesn’t require you to avoid the situation. Research shows ACT creates lasting improvements because you develop skills to handle future challenges rather than just reducing current symptoms.
“You can’t stop the waves, but you can learn to surf.”
Who it is for
ACT works well if you’ve spent years trying to control or eliminate uncomfortable emotions without success. This approach suits you if traditional CBT feels too focused on challenging thoughts when you need help living with them instead. You’ll benefit if your depression or anxiety has caused you to abandon important life areas like relationships, career goals, or hobbies. ACT helps people who feel stuck in rumination or worry loops that steal attention from the present moment.
What to expect from sessions
Sessions blend discussion with experiential exercises that help you practice new ways of relating to thoughts and emotions. Your therapist might use metaphors, mindfulness practices, or behavioral experiments to illustrate ACT principles. You’ll identify your personal values and create action plans that move you toward them. Homework typically includes mindfulness practice and values-based activities you complete between sessions. Most people attend 12 to 16 weekly sessions, though the timeline adjusts based on your progress.
Cost and access
ACT therapists practice in community mental health settings, private practices, and medical centers across the country. Psychologists and licensed therapists with specialized ACT training provide this treatment. Session costs range from $90 to $220 depending on your location and the therapist’s credentials. Insurance coverage follows standard mental health benefits, though you should confirm ACT-specific coverage with your plan. Many therapists now offer telehealth ACT sessions, making this approach accessible regardless of where you live.
5. Dialectical behavior therapy
Dialectical behavior therapy (DBT) was originally developed to treat borderline personality disorder, but therapists now use it successfully for depression and anxiety, especially when emotional intensity feels overwhelming. This therapy for depression and anxiety teaches you practical skills to manage intense emotions, tolerate distress, and improve relationships. DBT balances two seemingly opposite ideas: accepting yourself as you are while simultaneously working to change behaviors that cause problems. The “dialectical” part means you learn to hold both truths at once rather than swinging between extremes.
How it works
DBT combines individual therapy sessions with skills training groups where you learn four core modules: mindfulness, distress tolerance, emotion regulation, and interpersonal effectiveness. Your individual therapist helps you apply these skills to specific problems in your life. Between sessions, you track your emotions and behaviors on diary cards that guide treatment focus. Phone coaching gives you support when you’re practicing skills in real situations, not just talking about them in an office. The structured approach means you know exactly what to work on each week.
How it helps depression and anxiety
Depression often involves emotional numbness or overwhelming sadness that DBT’s emotion regulation skills help you navigate without making things worse. You learn to identify and name emotions, understand what triggers them, and reduce vulnerability to emotional swings through self-care basics. For anxiety, distress tolerance skills give you healthy ways to handle panic without resorting to avoidance or harmful coping methods. DBT helps when your emotions feel so intense that they drive impulsive decisions you regret later.
“You can’t stop the storm, but you can learn to dance in the rain without getting swept away.”
Who it is for
DBT works best if you experience intense emotional reactions that feel out of proportion to situations. You’ll benefit if your depression includes self-harm thoughts or behaviors that require immediate, practical coping strategies. This approach helps when anxiety causes panic attacks or overwhelming urges to escape situations. DBT suits you if previous therapy felt too abstract and you need concrete skills you can practice daily.
What to expect from sessions
You attend weekly individual therapy sessions lasting 50 minutes plus a 2-hour skills training group each week. Individual sessions focus on applying skills to your specific challenges and reviewing your diary cards. Groups teach new skills through lectures, practice, and homework assignments. Most people commit to at least six months of DBT, though a full course runs one year. Phone coaching between sessions provides real-time support when you’re struggling to use skills.
Cost and access
DBT programs operate in community mental health centers, hospitals, and private practices nationwide. Comprehensive DBT with both individual and group components costs $150 to $300 weekly when paying out of pocket. Insurance typically covers DBT under standard mental health benefits, though group sessions may have different coverage than individual therapy. Finding a full DBT program takes more effort than standard therapy since therapists need specialized training and certification. Some areas offer DBT skills groups without individual therapy at lower cost.
6. Interpersonal therapy
Interpersonal therapy (IPT) focuses on your relationships and life changes as the key to understanding and treating depression and anxiety. This therapy for depression and anxiety recognizes that mental health struggles often emerge from or worsen due to conflicts with others, grief, role transitions, or social isolation. Rather than exploring your childhood or deep personality patterns, IPT concentrates on your current relationships and recent life events. The approach typically runs for a defined period with clear goals related to improving how you connect with others.
How it works
Your therapist helps you identify one or two interpersonal problem areas causing distress: grief over loss, disputes with significant people in your life, difficult life transitions, or social isolation. Sessions focus on understanding how these relationship challenges connect to your depression or anxiety symptoms. You’ll explore communication patterns that create problems and practice new ways of expressing needs or resolving conflicts. IPT treats symptoms by improving the quality of your relationships rather than by changing thought patterns or behaviors directly.
How it helps depression and anxiety
Depression often develops when relationships feel unsatisfying or when major life changes disrupt your sense of identity and connection. IPT helps you process losses, negotiate relationship changes, and build stronger social support, which naturally reduces depressive symptoms. For anxiety, the therapy addresses worries rooted in relationship conflicts or fear of social judgment. You learn to communicate more effectively, reducing the interpersonal stress that fuels anxious thoughts.
“Your mental health improves when your relationships improve, because we’re fundamentally social creatures who need connection to thrive.”
Who it is for
IPT works well if you can identify specific relationship problems or life changes that preceded or worsened your symptoms. You’ll benefit if your depression stems from grief, divorce, job changes, or conflicts with family or partners. This approach suits people who prefer focusing on present relationships rather than past experiences or thought patterns. IPT helps when you feel isolated or when important relationships cause more stress than support.
What to expect from sessions
Sessions last 50 minutes and follow a structured timeline of 12 to 16 weeks. Your therapist starts by taking a detailed interpersonal inventory of your significant relationships and recent life events. Each session focuses on relationship issues from the previous week, exploring what happened and how you might handle similar situations differently. You’ll practice communication skills and develop strategies for specific relationship challenges.
Cost and access
IPT therapists work in private practices, hospital systems, and community mental health centers. Psychologists and clinical social workers with specialized IPT training provide this treatment. Session costs range from $90 to $200 without insurance. Most insurance plans cover IPT under standard mental health benefits. You can find IPT therapists through referrals from your primary care doctor or by searching mental health provider directories.
7. EMDR therapy
Eye Movement Desensitization and Reprocessing (EMDR) therapy works differently from traditional talk therapy by helping your brain reprocess traumatic memories that fuel depression and anxiety. When you experience trauma, your brain sometimes stores the memory incorrectly, keeping it emotionally raw and present rather than filed away as something that happened in the past. This therapy for depression and anxiety uses bilateral stimulation, like guided eye movements, to help your brain finish processing these stuck memories so they lose their emotional charge.

How it works
Your therapist guides you through eight phases of treatment, starting with history-taking and preparation before moving to memory reprocessing. During reprocessing sessions, you briefly focus on a distressing memory while simultaneously following your therapist’s finger movements with your eyes or experiencing other bilateral stimulation like tapping. This dual attention allows your brain to process the memory without becoming overwhelmed, connecting it with more adaptive information stored elsewhere in your brain. The process continues until the memory no longer triggers intense emotional reactions.
How it helps depression and anxiety
Depression often stems from traumatic experiences that left you feeling helpless, worthless, or hopeless. EMDR helps by reprocessing these core memories so they stop reinforcing negative beliefs about yourself. For anxiety, this therapy addresses the hyperarousal and fear responses that persist long after threats have passed. Your nervous system learns that the danger is over, reducing constant vigilance and worry.
“EMDR allows your brain to heal from psychological trauma much like your body recovers from physical wounds.”
Who it is for
EMDR works well if you’ve experienced specific traumatic events like accidents, assault, or sudden losses that now trigger depression or anxiety. You’ll benefit if intrusive memories or flashbacks disrupt your daily life. This approach helps when talking about trauma feels too overwhelming or when traditional therapy hasn’t provided relief.
What to expect from sessions
Sessions last 60 to 90 minutes to allow time for complete reprocessing. Your therapist teaches you self-soothing techniques before starting memory work. Treatment typically requires 6 to 12 sessions, though complex trauma may need more. You might feel emotionally tired after sessions as your brain continues processing.
Cost and access
EMDR therapists practice in private offices, trauma centers, and hospitals nationwide. Session costs range from $100 to $250 depending on location and credentials. Insurance typically covers EMDR under standard mental health benefits. Trellis Counseling offers EMDR as part of their trauma-informed services.
8. Internal Family Systems therapy
Internal Family Systems (IFS) therapy views your psyche as containing multiple “parts” or subpersonalities that developed to protect you from pain and help you survive difficult experiences. This therapy for depression and anxiety recognizes that what feels like internal conflict reflects different parts of you with competing needs. One part might push you to achieve while another wants you to stay safe by avoiding risk. IFS helps you understand these parts, appreciate their protective intentions, and access your core Self, which naturally holds qualities like compassion, curiosity, and confidence.
How it works
Your therapist helps you identify the different parts inside you, such as a critical inner voice, an anxious protector, or a vulnerable younger part carrying old wounds. You learn to approach these parts with curiosity rather than judgment, asking what they’re trying to protect you from and what they need from you. IFS distinguishes between managers (parts that try to control situations), firefighters (parts that react to overwhelming emotions), and exiles (vulnerable parts holding painful memories). Through guided exercises, you access your core Self to lead these parts rather than being led by them.
How it helps depression and anxiety
Depression often involves parts that feel hopeless or worthless taking over your entire sense of self. IFS helps you recognize these as just parts of you, not your whole identity, creating space for healing. For anxiety, this approach addresses the protective parts that developed hypervigilance to keep you safe but now cause constant worry. You help these parts relax by showing them that your Self can handle challenges they’ve been trying to manage alone.
“You’re not broken or defective. You simply have parts that are stuck in the past, trying to protect you from dangers that no longer exist.”
Who it is for
IFS works well if you experience internal conflict or notice competing voices in your head that create paralysis. You’ll benefit if you’ve felt like different parts of yourself want contradictory things. This approach helps when you recognize younger, wounded parts of yourself that need attention and compassion.
What to expect from sessions
Sessions last 50 to 60 minutes and involve guided exploration of your internal system. Your therapist asks questions that help you notice and communicate with different parts. Treatment typically requires 12 to 20 sessions, though complex trauma may need longer.
Cost and access
IFS therapists practice in private offices and trauma treatment centers across the country. Session costs range from $100 to $250 depending on location. Insurance covers IFS under standard mental health benefits. Trellis Counseling offers IFS as part of their trauma-informed approach.
9. Exposure therapy
Exposure therapy confronts the avoidance patterns that maintain anxiety and depression by gradually helping you face feared situations, objects, or memories. This therapy for depression and anxiety works on the principle that avoiding what scares you provides temporary relief but strengthens fear long-term. When you systematically face feared situations in a controlled way, your brain learns that the danger you anticipated doesn’t materialize or that you can handle it better than expected. The approach requires courage but produces lasting changes in how you respond to triggers.
How it works
Your therapist creates a hierarchy of feared situations ranked from least to most anxiety-provoking. You start with exposures that cause manageable discomfort and gradually work up to more challenging scenarios. During exposures, you stay in the situation until your anxiety naturally decreases, teaching your nervous system that the threat isn’t real or as dangerous as your mind predicts. Exposures happen in imagination, through virtual reality, or in real-world settings depending on what you’re avoiding. Your therapist stays with you during initial exposures, helping you resist safety behaviors that prevent full learning.
How it helps depression and anxiety
Anxiety disorders thrive on avoidance, which shrinks your life and confirms your fears about what you can’t handle. Exposure therapy breaks this cycle by proving that feared outcomes rarely happen and that temporary discomfort is manageable. For depression linked to avoidance, facing situations you’ve been dodging rebuilds confidence and reconnects you with meaningful activities. Research shows exposure creates neurological changes that reduce fear responses permanently rather than just temporarily.
“Courage isn’t the absence of fear. It’s taking action despite fear and discovering you’re stronger than you believed.”
Who it is for
Exposure therapy works best if you have specific phobias, panic disorder, social anxiety, or post-traumatic stress disorder with clear avoidance patterns. You’ll benefit if your world has narrowed significantly due to avoiding certain places, people, or situations. This approach helps when you recognize that avoidance controls your choices and limits your life.
What to expect from sessions
Sessions last 60 to 90 minutes to allow time for complete exposures. Your therapist guides you through planned exposures while tracking your anxiety levels. Treatment typically requires 8 to 15 sessions depending on the number of fears you’re addressing.
Cost and access
Exposure therapy specialists work in anxiety disorder clinics, private practices, and hospital programs nationwide. Session costs range from $100 to $250 without insurance. Most insurance plans cover exposure therapy under standard mental health benefits.
10. Mindfulness-based cognitive therapy
Mindfulness-based cognitive therapy (MBCT) combines meditation practices with cognitive therapy principles to prevent depression relapse and reduce anxiety symptoms. This therapy for depression and anxiety teaches you to notice thoughts and feelings without getting caught up in them or trying to change them immediately. MBCT recognizes that rumination patterns keep you stuck in negative thinking cycles. The approach gives you tools to observe your mental activity from a distance, creating space between you and your thoughts so they lose their power over your mood and actions.

How it works
MBCT teaches you mindfulness meditation techniques that help you pay attention to present-moment experiences without judgment. You learn to notice when your mind wanders into past regrets or future worries, then gently return focus to your breath or body sensations. The cognitive component helps you recognize warning signs that depression might be returning, such as specific thought patterns or physical tension. You practice relating differently to these early signals rather than trying to push them away or fix them immediately.
How it helps depression and anxiety
Depression often involves getting lost in negative thought spirals about yourself, your life, or your future. MBCT helps you step back from these thoughts and see them as mental events rather than facts. For anxiety, this approach reduces the power of worrying by teaching you to observe anxious thoughts without engaging with their content or predictions. Research shows MBCT cuts depression relapse rates in half for people who’ve experienced multiple episodes.
“Thoughts are just thoughts. They’re not facts, commands, or predictions that require your immediate response.”
Who it is for
MBCT works well if you’ve experienced recurrent depression and want to prevent future episodes. You’ll benefit if your mind constantly jumps to past mistakes or future catastrophes. This approach helps when you find yourself overthinking situations or struggling to stay present in daily activities.
What to expect from sessions
Sessions last 2 to 2.5 hours and include guided meditation practice, group discussion, and education about depression patterns. Treatment follows an 8-week structured program with daily home practice requirements of 45 minutes. You attend weekly group sessions with 8 to 15 other participants.
Cost and access
MBCT programs operate in hospitals, mental health centers, and meditation centers across the country. Eight-week programs cost $300 to $600 total when paying out of pocket. Insurance coverage varies since MBCT often runs as a group education program rather than traditional therapy.
11. Problem-solving therapy
Problem-solving therapy (PST) treats depression and anxiety by teaching you practical skills to address the real-life challenges that trigger or worsen your symptoms. This therapy for depression and anxiety recognizes that stress from unsolved problems creates a sense of helplessness that fuels mental health struggles. Rather than focusing on emotions or thoughts alone, PST gives you a structured method for tackling difficulties in relationships, work, health, or daily responsibilities. The approach works on the principle that improving your problem-solving abilities reduces stress and builds confidence in handling future challenges.
How it works
Your therapist teaches you a systematic problem-solving process with clear steps: defining the problem accurately, brainstorming possible solutions without judging them, evaluating the pros and cons of each option, choosing one to try, and reviewing the results. You learn to break down overwhelming situations into manageable pieces that feel less intimidating. PST helps you distinguish between problems you can solve and situations you need to accept. Your therapist guides you through applying this framework to specific current problems rather than just discussing the process theoretically.
How it helps depression and anxiety
Depression often stems from feeling overwhelmed by accumulated unsolved problems that seem insurmountable. PST breaks this pattern by helping you tackle issues one at a time, building momentum and reducing hopelessness. For anxiety, this approach addresses the paralysis that comes from worrying about problems without taking action. You replace anxious rumination with productive problem-solving steps, giving your mind something constructive to do with its energy.
“The best way out is always through. Problem-solving therapy gives you the map.”
Who it is for
PST works well if your depression or anxiety worsens when you face specific life stressors like financial difficulties, relationship conflicts, or work challenges. You’ll benefit if you tend to avoid problems or feel overwhelmed when multiple issues pile up at once. This approach helps people who want practical solutions rather than emotional exploration.
What to expect from sessions
Sessions last 50 minutes and focus on applying the problem-solving framework to your current challenges. Your therapist helps you work through actual problems you’re facing right now. Treatment typically requires 6 to 12 weekly sessions depending on the complexity of issues you’re addressing.
Cost and access
PST practitioners work in community mental health centers, primary care offices, and private practices nationwide. Session costs range from $80 to $180 without insurance. Most insurance plans cover PST under standard mental health benefits, making this accessible treatment available to many people.
12. Couples therapy for anxiety and depression
Couples therapy recognizes that relationship dynamics significantly impact individual mental health, and your partner’s involvement can accelerate recovery from depression and anxiety. This therapy for depression and anxiety treats the relationship as a system where each person’s emotions and behaviors affect the other. When one partner struggles with mental health challenges, the relationship often develops strained communication patterns that worsen symptoms for both people. Working together in therapy breaks destructive cycles and builds mutual understanding that supports healing.
How it works
Your therapist helps both partners understand how depression or anxiety symptoms affect relationship interactions and vice versa. Sessions explore communication breakdowns, assumptions each person makes about the other’s behavior, and patterns that maintain distress. You learn to express needs more clearly and respond to your partner with empathy rather than criticism or withdrawal. The therapist might assign homework where you practice new interaction patterns between sessions, such as scheduling quality time together or using specific communication techniques during conflicts.
How it helps depression and anxiety
Depression in one partner often creates distance and misunderstandings that leave both people feeling isolated. Couples therapy helps your partner understand that your withdrawal reflects illness rather than rejection, reducing conflict that deepens depression. For anxiety, having your partner’s support in facing fears makes exposures less overwhelming. You develop shared strategies for managing panic attacks or anxious moments together rather than letting anxiety divide you.
“Your relationship can be either a refuge that supports healing or a source of stress that worsens symptoms. Couples therapy transforms it into the former.”
Who it is for
This approach works when your depression or anxiety strains your relationship or when relationship problems trigger symptoms. You’ll benefit if your partner wants to help but doesn’t know how or if misunderstandings about your symptoms create recurring conflicts. Couples therapy helps when you both feel stuck in negative patterns that neither person knows how to break.
What to expect from sessions
Sessions last 50 to 75 minutes with both partners present. Your therapist creates space for each person to share their experience while teaching constructive communication skills. Treatment typically requires 8 to 16 weekly sessions, though some couples continue longer for complex issues.
Cost and access
Couples therapists practice in private offices, relationship counseling centers, and mental health clinics nationwide. Session costs range from $100 to $300 depending on location and therapist credentials. Insurance coverage varies since some plans treat couples therapy differently than individual therapy, so verify your specific benefits before starting.
Next steps
Finding the right therapy for depression and anxiety takes courage, and you’ve already taken an important step by learning about your options. No single approach works for everyone, which means you might need to try different methods before discovering what helps you most. The therapies outlined here have strong research backing, and many people combine elements from multiple approaches to address their specific needs.
Your path forward starts with reaching out to a qualified therapist who can assess your situation and recommend the best starting point. If you’re in Oregon and dealing with depression or anxiety rooted in traumatic experiences, Trellis Counseling offers trauma-informed care that integrates several evidence-based approaches. Their therapists specialize in helping people rebuild their lives after difficult experiences, whether recent or long past.
Don’t let another day pass feeling stuck in depression or paralyzed by anxiety. Contact Trellis Counseling to schedule an initial consultation and begin your journey toward feeling like yourself again.